Starved T cells allow hepatitis B to silently infect liver
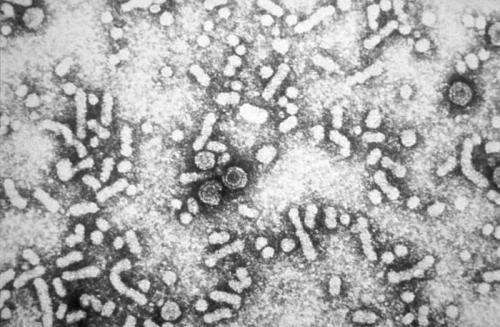
Hepatitis B stimulates processes that deprive the body's immune cells of key nutrients that they need to function, finds new UCL-led research funded by the Medical Research Council and Wellcome Trust.
The work helps to explain why the immune system cannot control hepatitis B virus infection once it becomes established in the liver, and offers a target for potential curative treatments down the line. The research also offers insights into controlling the immune system, which could be useful for organ transplantation and treating auto-immune diseases.
Worldwide 240 million people have chronic hepatitis B and 780,000 people die each year from the liver cirrhosis and cancer that it causes; existing treatments can rarely cure this infection. A preventative vaccination against the virus is available, however it is not routinely given in the UK and is of no use once you have the infection. Liver disease is the only major cause of premature death currently increasing in the UK, and hepatitis B and C are the second commonest underlying causes after alcohol.
Most adults' immune systems can control hepatitis B virus within a year (acute infection), but chronic infection is common in children, particularly in newborns whose mothers carry the virus, and lasts a lifetime. The new study, published in Nature Medicine, suggests that hepatitis B can persist by taking advantage of suppressor cells in the liver that starve immune responses to silence them.
"Hepatitis B patients usually don't have symptoms for decades, so can carry the virus unknowingly and can spread it through childbirth, sexual contact or contaminated needles," says senior author Professor Mala Maini (UCL Infection & Immunity). "Our work has shown that during this 'silent phase' of infection, specialised suppressor cells switch off the immune response by cutting off its food supply. This is one of the many ways the liver protects itself from inflammation and immune damage but at the same time, prevents elimination of pathogens like hepatitis B.
"If we could boost the immune system and counteract the liver's suppressive effect, then the infection could potentially be cleared after a large 'burst' of immune activity. This might cause short-term damage to the liver, but would prevent the long-term damage from scarring and liver cancers that we see in chronic patients."
The team compared blood samples from 138 chronic hepatitis B patients and 99 healthy controls, and examined liver tissue samples from 42 patients. They found that patients in the silent phases of infection had high levels of cells called granulocytic myeloid-derived suppressor cells (gMDSCs). These gMDSCs, which suppress T cells (immune cells) by cutting off their food supply, were found to accumulate in the liver.
"The gMDSCs suppressed both the T cells that fight hepatitis B virus and those that cause inflammation in the liver," explains lead author Dr Laura Pallett (UCL Infection & Immunity). "So patients with more gMDSC tended to have less liver damage but were unable to control hepatitis B virus. Women had higher levels of gMDSC than men, which fits with their threefold lower risk of developing liver inflammation from hepatitis B."
These findings emphasise how nutrient supplies can regulate the immune system. They also suggest that suppressor cells such as gMSDC might have clinical uses in cases where the immune system attacks healthy tissue, such as autoimmune diseases or immune rejection of donated organs.
"If these cells can prevent immune cells from damaging the liver in hepatitis B patients, perhaps they could help to prevent immune rejection of transplanted livers," says Professor Maini. "Similarly, such suppressor cells could potentially be harnessed to protect specific organs from damage in patients with autoimmune diseases."
More information: Metabolic regulation of hepatitis B immunopathology by myeloid-derived suppressor cells, DOI: 10.1038/nm.3856