Researchers identify molecular link between schizophrenia and diabetes risk
It has long been known that psychiatric disorders, such as schizophrenia, have been associated with a higher risk of type 2 diabetes. In a new study published online in The FASEB Journal, a UMass Medical School research team, led by Rita Bortell, PhD, research professor of molecular medicine and Agata Jurczyk, PhD, instructor in molecular medicine, found that a shared gene (or genes) may underlie the co-occurrence of both diseases. Mutations in Disrupted in Schizophrenia 1 (DISC1) have been strongly associated with major psychiatric disorders, including schizophrenia, but not diabetes. This study presented the first evidence to indicate that the DISC1 gene also plays a novel, unexpected role in pancreatic beta cell survival and function. It is also the first to provide a molecular link for a prevalence of type 2 diabetes in individuals with psychiatric disorders.
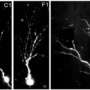
To make this discovery, Dr. Bortell and her team genetically manipulated a group of mice to disrupt the DISC1 gene only in the mouse's pancreatic beta cells, not in the brain. The mice with the disrupted DISC1 gene showed an increase in beta cell death, less insulin secretion and impaired glucose regulation compared to normal mice. When these researchers studied cultured beta cells in which DISC1 expression was suppressed, they found that DISC1 works by inhibiting the activity of a specific protein, GSK3β. Lowered GSK3β activity was already known to be critical for beta cell function and survival. The research team further tested the validity of this association by inhibiting GSK3β function directly. This resulted in improved beta cell survival and restored normal glucose tolerance in mice with disrupted DISC1. These results uncover an unexpected role for DISC1 in normal beta cell physiology and suggest that DISC1 may regulate blood glucose independently of its function in the brain.
"It is known that individuals with psychiatric disorders may be predisposed to developing type 2 diabetes due to several interacting factors including genetics, lifestyle and medications. Based on our mouse studies, our data predict that DISC1 disruption could tip the balance toward disease," Bortell said, adding that it remains to be demonstrated in humans. "Our hope is that the association we've found linking disrupted DISC1 to both diabetes and psychiatric disorders may uncover mechanisms to improve therapies to alleviate suffering caused by both illnesses, which are extraordinarily costly, very common and quite debilitating."
Bortell said the study points out the potential importance of evaluating new antipsychotic medications for their effects on pancreatic beta cells in addition to the brain. Diligent monitoring for diabetes in those with psychiatric disorders is further warranted by the fact that many antipsychotic medications are also associated with an increased risk of diabetes. "We are also intrigued by the fact that diabetic individuals have higher rates of depression, which suggests that additional molecular links in brain and pancreatic beta cells may yet be discovered," Bortell said.
The full study can be found online in The FASEB Journal and will be published in print in February.
More information: A. Jurczyk et al. Beyond the brain: disrupted in schizophrenia 1 regulates pancreatic -cell function via glycogen synthase kinase-3 , The FASEB Journal (2015). DOI: 10.1096/fj.15-279810