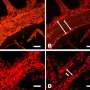
The immune system of mice is implicated in helping malaria to move from the blood to the brain
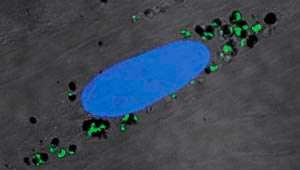
By studying malaria in mice, three A*STAR researchers have discovered how malaria parasites in the bloodstream can affect the brain, causing a life-threatening condition called cerebral malaria.
Cerebral malaria is a complication that arises from the most dangerous form of the blood disease. It is the main cause of death from malaria and kills hundreds of thousands of children in Africa every year.
Since malaria is a blood-borne disease, the brain should be isolated from it by the blood–brain barrier, which restricts the transfer of certain compounds from the blood to the brain. It was not clear how this barrier is breached in cases of cerebral malaria.
Now, Shanshan Howland, Chek Meng Poh and Laurent Rénia of the Singapore Immunology Network have shown how malaria breaks through the blood–brain barrier in mice.
They discovered that cells that line the blood vessels, known as endothelial cells, take up material from malaria-infected red blood cells coursing through the blood vessels in the mice's brains. These endothelial cells then 'display' small fragments of proteins (peptides) derived from the parasite on their surfaces (see image). This means the peptides act as targets for the body's immune system, which mistakes them for parasitic cells. In particular, they are attacked by immune cells known as killer T cells, and in this way the blood–brain barrier is broken down, often with fatal results.
A similar process may occur in humans ― the researchers showed that endothelial cells from the human brain grown in culture also take up malarial parasites in a similar way. But to conclusively prove this connection will require ascertaining whether there are any equivalent peptides with the same function in humans.
The finding has the potential to save lives. "Right now, the only treatment available is anti malarial drugs to kill the parasites, and the mortality rate in African children can be around 20 per cent even with treatment. Children often die within a day or two of entering hospital," says Howland. "If we can block presentation of peptides by endothelial cells or the immune recognition of such, it could buy time for anti malarials to clear the parasites."
The discovery is significant for other serious neurological diseases besides cerebral malaria. "The ability to display peptides from pathogens is generally restricted to specialized immune cells, but our study has shown for the first time that brain endothelial cells can also do the same," explains Howland. "This has important implications for multiple sclerosis, encephalitis and meningitis."
More information: Shanshan W. Howland et al. Activated Brain Endothelial Cells Cross-Present Malaria Antigen, PLOS Pathogens (2015). DOI: 10.1371/journal.ppat.1004963