Researchers discover how breast cancer mutation in BRCA1 causes protein to self-destruct

Of the more than 3 million people with breast cancer in the United Stated, about 10 percent carry an inherited mutation in their BRCA1 gene. In health, the gene is responsible for suppressing tumors. In disease, the gene goes terribly awry.
Scientists at the Virginia Tech Carilion Research Institute found that breast cancer cells can trigger the self-destruction of the tumor-suppressing BRCA1 proteins. They published their results today (Feb. 28) in Scientific Reports, a Nature journal.
"There are different ways in which DNA damage can be repaired. The breast cancer susceptibility protein, BRCA1, has an interesting mechanism as a tumor suppressor," said Deborah Kelly, an assistant professor at the Virginia Tech Carilion Research Institute and senior author on the paper. "Unfortunately, where there are mutations in BRCA1, there's a significant decrease in its ability to repair DNA and cells are more likely to become cancerous."
Scientists knew the mutations promoted cancer, but they didn't know exactly how BRCA1 physically changed, or how those changes prevented the protein from participating in DNA repair.
Kelly and her team focused on a highly prevalent BRCA1 mutation to begin to understand not only the structural changes, but also the functional fallout. Using molecular imaging and biochemical tools, the researchers examined human cancer cells and found that mutated BRCA1 proteins were destroyed under stressful, oxidative cellular conditions. The proteins were unable to properly repair damaged DNA.
"The system we use mimics the chain of events resulting from the inappropriate breakdown of estrogen, which produces molecules known as reactive oxygen species that can modify DNA and proteins, contributing to cancer," Kelly said.
Healthy cells can manage the damage caused by reactive oxygen species, also called free radicals, with repair proteins. Kelly and her team saw that typical BRCA1 proteins remained relatively stable, but mutated BRCA1 proteins significantly reduced in number.
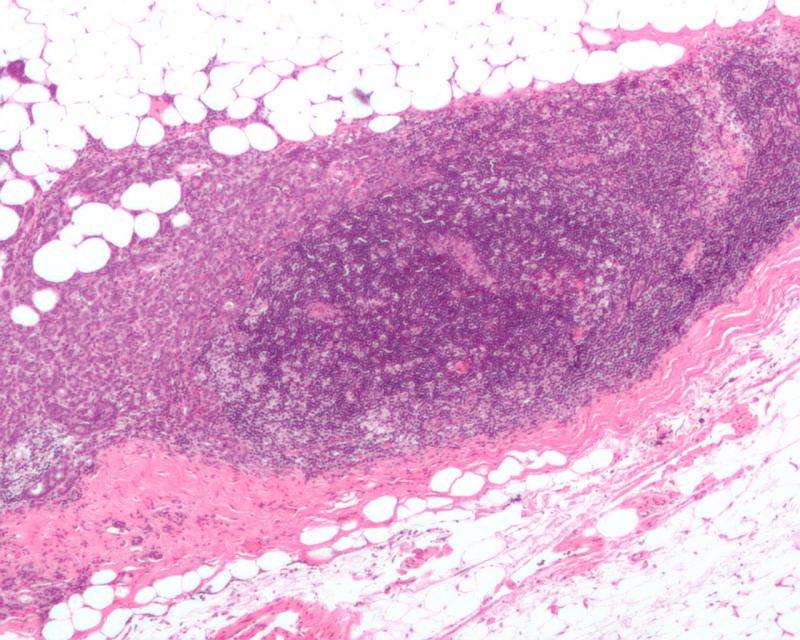
Cells tag the mutated BRCA1 protein for destruction with a molecule called ubiquitin, according to Kelly. The cells then destroy the ubiquitin-tagged BRCA1 proteins, leading to a decrease in their ability to repair DNA lesions.
Kelly and her team are not the first to identify ubiquitination, but they are the first to recognize that the process increases in response to the BRCA1 mutation. They suspect that the BRCA1 mutation causes a small misfolding that allows even more ubiquitin to attach to the protein.
"Some ubiquitin modifications actually enhance the function of proteins, but, in this case, it acts as a target for degradation," said Kelly, who is also an assistant professor of biological sciences at Virginia Tech's College of Science. "Compared with non-mutated BRCA1 proteins, the ubiquitination process heightens the destruction of mutated BRCA1 proteins. The levels are lowered to a point where its power to assist in genomic maintenance is compromised."
The process of ubiquitation is already a target for a potential therapeutic treatment, according to Kelly. It's theoretically possible for enzymes to block or remove the ubiquitin, allowing cells to potentially enhance or restore BRCA1's function as a tumor suppressor.
"We demonstrated that protein levels, genetic mutations, and the chemical changes in proteins after they are made, known as post-translational modifications - particularly ubiquitination - can affect BRCA1's functional state in breast cancer cells," Kelly said. "Based on the results of this work, the next logical step is to test mechanistic-based therapies, such as enzymes that remove ubiquitin to restore the physical properties of the mutated BRCA1."
Current experiments in the Kelly Lab involve determining the 3D structures of healthy and mutated BRCA1 using high resolution cryo-electron microscopy.
This information may help scientists more fully understand the extent to which some individuals with BRCA1 mutations are more disposed to cancer than others, based on physical changes to the BRCA1 protein structure.
More information: Scientific Reports, DOI: 10.1038/srep43435