Cancer immunotherapy may work in unexpected way
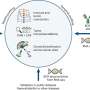
Antibodies to the proteins PD-1 and PD-L1 have been shown to fight cancer by unleashing the body's T cells, a type of immune cell. Now, researchers at the Stanford University School of Medicine have shown that the therapy also fights cancer in a completely different way, by prompting immune cells called macrophages to engulf and devour cancer cells.
The finding may have important implications for improving and expanding the use of this cancer treatment, the researchers said.
A study describing the work, which was done in mice, was published online May 17 in Nature. The senior author is Irving Weissman, MD, professor of pathology and of developmental biology. The lead author is graduate student Sydney Gordon.
PD-1 is a cell receptor that plays an important role in protecting the body from an overactive immune system. T cells, which are immune cells that learn to detect and destroy damaged or diseased cells, can at times mistakenly attack healthy cells, producing autoimmune disorders like lupus or multiple sclerosis. PD-1 is what's called an "immune checkpoint," a protein receptor that tamps down highly active T cells so that they are less likely to attack healthy tissue.
How cancer hijacks PD-1
About 10 years ago, researchers discovered that cancer cells learn to use this immune safeguard for their own purposes. Tumor cells crank up the production of PD-L1 proteins, which are detected by the PD-1 receptor, inhibiting T cells from attacking the tumors. In effect, the proteins are a "don't kill me" signal to the immune system, the Stanford researchers said. Cancer patients are now being treated with antibodies that block the PD-1 receptor or latch onto its binding partner, PD-L1, to turn off this "don't kill me" signal and enable the T cells' attack.
"Using antibodies to PD-1 or PD-L1 is one of the major advances in cancer immunotherapy," said Weissman, who is also the Virginia and D.K. Ludwig Professor for Clinical Investigation in Cancer Research, director of the Stanford Institute for Stem Cell Biology and Regenerative Medicine and director of the Ludwig Center for Cancer Stem Cell Research and Medicine at Stanford. "While most investigators accept the idea that anti-PD-1 and PD-L1 antibodies work by taking the brakes off of the T-cell attack on cancer cells, we have shown that there is a second mechanism that is also involved."
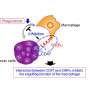
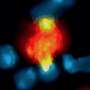
What Weissman and his colleagues discovered is that PD-1 activation also inhibits the anti-cancer activity of other immune cells called macrophages. "Macrophages that infiltrate tumors are induced to create the PD-1 receptor on their surface, and when PD-1 or PD-L1 is blocked with antibodies, it prompts those macrophage cells to attack the cancer," Gordon said.
Similar to anti-CD47 antibody
This mechanism is similar to that of another antibody studied in the Weissman lab: the antibody that blocks the protein CD47. Weissman and his colleagues showed that using anti-CD47 antibodies prompted macrophages to destroy cancer cells. The approach is now the subject of a small clinical trial in human patients.
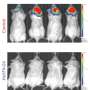
As it stands, it's unclear to what degree macrophages are responsible for the therapeutic success of the anti-PD-1 and anti-PD-L1 antibodies.
The practical implications of the discovery could be important, the researchers said. "This could lead to novel therapies that are aimed at promoting either the T-cell component of the attack on cancer or promoting the macrophage component," Gordon said.
Another implication is that antibodies to PD-1 or PD-L1 may be more potent and broadly effective than previously thought. "In order for T cells to attack cancer when you take the brakes off with antibodies, you need to start with a population of T cells that have learned to recognize specific cancer cells in the first place," Weissman said. "Macrophage cells are part of the innate immune system, which means they should be able to recognize every kind of cancer in every patient."
More information: Sydney R. Gordon et al. PD-1 expression by tumour-associated macrophages inhibits phagocytosis and tumour immunity, Nature (2017). DOI: 10.1038/nature22396