Sequencing prostate tumors from African-American men reveals a novel tumor suppressor gene
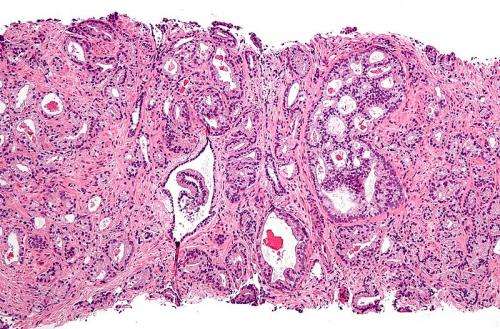
African-American men develop prostate cancer more often than other men, and it tends to be more deadly for this population. Some of the differences seem to be due to socioeconomic factors, but scientists wondered whether the disparities are also rooted in the tumor genome.
To explore whether racial disparities in prostate cancer incidence and prognosis stem from molecular and genetic differences, a team of researchers at the Broad Institute of MIT and Harvard including Broad institute member Levi Garraway and postdoctoral researcher Franklin Huang gathered tumor samples from 102 African-American men with prostate cancer and analyzed their exomes. The work appears in Cancer Discovery.
After sequencing the exomes (protein-coding portions of the genome) from these tumors and validating their results in another 90 patients, they uncovered several mutations not recognized before in this setting. Interestingly, they found that the gene ERF, which had never been implicated in any particular cancer, was mutated in 5 percent of the men in the study. ERF is a member of the ETS family of transcription factors, and rearrangements in other ETS family genes have been found in prostate cancer and are thought to drive cancer by turning other genes on. The genetic misspellings they found in ERF, however, are so-called "loss-of-function" mutations that effectively remove the function of the gene, demonstrating that ERF is a novel prostate cancer tumor suppressor gene that normally acts to slow cancer growth.
When they examined existing data on prostate cancer samples from other cohorts, such as The Cancer Genome Atlas (TCGA) project which includes people of mostly European descent, they observed that the ERF gene was deleted in 3 percent of primary prostate cancers and mutated or deleted in 3-5 percent of lethal prostate cancers that had become resistant to androgen-depleting therapy. The alterations in the TCGA samples weren't significant enough on their own to implicate ERF, but in light of the findings in the new study, support a role for the mutant gene in driving prostate cancer.
The researchers also found differences in other genes, including amplifications (present in multiple copies) and deletions, but more work remains to fully explain the disparity in prostate cancer incidence and severity among patients of different ancestries. Because prostate cancer has a relatively low mutation rate compared to other cancers, many more samples may be needed. The scientists plan to look for genetic differences among larger groups of African-Americans, and to also study patients native to West Africa, a region in which African-Americans tend to have ancestry.
The success of this effort in uncovering subtle genomic differences and revealing a new prostate cancer gene demonstrates the power of including diverse populations in genetic analyses. Discoveries made from studying patients of diverse ethnic backgrounds can shed light on the underlying biology of this disease for all patients.
More information: Franklin W. Huang et al. Exome Sequencing of African-American Prostate Cancer Reveals Loss-of-FunctionMutations, Cancer Discovery (2017). DOI: 10.1158/2159-8290.CD-16-0960


















