Cellular stress increases the probability of developing autoimmune diseases
A team of researchers led by Marc Veldhoen at the Instituto de Medicina Molecular (iMM), Lisboa, has found that cellular stress enhances the activation of immune cells implicated in many chronic inflammatory conditions, increasing the risk of autoimmune diseases.
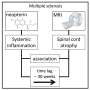
T cells, a type of white blood cell, can be tuned into different activation modes, thereby tailoring immune responses to adequately deal with infections. However, some of these activation modes particularly contribute to autoimmune diseases such as arthritis, diabetes and multiple sclerosis.
The Veldhoen lab has studied T cell activation modes for many years, and the researchers previously observed that one particular activation status, termed Th17, is much more robust than other states, leading them to hypothesize that these cells are more resistant to adverse conditions than other T cell counterparts.
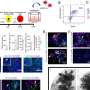
By controlling external conditions such as osmotic pressure, sugar concentration in the culture medium, and oxygen pressure, the team discovered that Th17 cells are preferentially generated under adverse conditions when compared to optimal conditions. Moreover, by using mouse models of autoimmunity, Veldhoen and colleagues demonstrated that if cell stress was inhibited, lower numbers of Th17 cells were generated, and the animals had reduced disease symptoms.
There has been an increasing focus from both academia and pharmaceutical companies in recent years on Th17 cells, since they are implicated in several chronic inflammatory conditions. In fact, studies interfering with the biology of these cells have shown promise for therapeutic applications in psoriasis and arthritis, for example.
These novel findings offer additional pharmacological targets to reduce cellular stress at sites of inflammation by reducing Th17 generation and preserving other T cell responses that may hold important clinical implications.
More information: Verena Brucklacher-Waldert et al. Cellular Stress in the Context of an Inflammatory Environment Supports TGF-?-Independent T Helper-17 Differentiation, Cell Reports (2017). DOI: 10.1016/j.celrep.2017.05.052