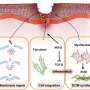
Mathematical models for healing burns
Daniël Koppenol, together with Fred Vermolen (both TU Delft), has developed various mathematical models to simulate the healing of wounds, in particular burns, with the aim of improving healing. As Vermolen points out, collaboration between the disciplines of mathematics, biology and medicine is still in its infancy, but it would offer great opportunities. Koppenol has been awarded a PhD for this work at TU Delft on Thursday, 15 June.
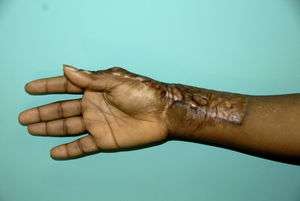
Hypertrophic scars
Daniël Koppenol's research focused among other things on hypertrophic scars: raised, often red and very tough scars that are painful and itchy and may reduce mobility. They are a very distressing complication of wounds, particularly burns, which is relative common in young people aged 20 to 30, particularly among dark-skinned people.
Substantial improvement
Although wound treatment has improved substantially in recent decades, it still does not result in complete regeneration of the affected skin, and leaves scar tissue. The presence of scar tissue may cause complications such as limited mobility in the affected skin. Also, large wounds often do not heal satisfactorily, resulting for example in a body part becoming misaligned (contracture) and hypertrophic scar tissue. 'Unfortunately, the underlying mechanisms of the development of contractures and hypertrophic scar tissue are not currently known,' says Koppenol. 'It is also difficult to influence the material properties of developing scar tissue. A better understanding of the mechanisms underlying wound healing would probably improve treatment.'
Mathematical models rather than experiments
A great deal of research has been done into these mechanisms, but unfortunately there is still a lot we do not know. This is due partly to the complexity of the wound healing process, but also to the fact that it is very difficult to study the interactions between the various process components in an experimental setting. This problem can be overcome by using mathematical models. Koppenol has developed models to simulate the healing of different types of wounds and the development of scars, thus helping to unravel the mechanisms behind normal and abnormal wound healing, in the process also offering perspectives for alternatives for animal testing.
Improve treatment
Once we have a better understanding of how wounds heal we can treat them better and thus minimise scarring. At present, for example, we do not know when splint therapy should ideally start after skin is grafted onto an excised burn wound so as to prevent contractures from developing. Based on the results from one of his models, Koppenol suggests that the ideal time to start splint therapy is immediately after the skin graft.
Koppenol explains: 'Our ultimate aim is to develop a versatile mathematical model capable of accurately simulating various aspects of the healing of different types of wounds, so as to help identify the mechanisms behind normal and abnormal wound healing and thus improve the treatment of both wounds and scars.'
More information: Biomedical implications from mathematical models for the simulation of dermal wound healing, repository.tudelft.nl/islandora/object/uuid%3Acdc7392f-4ac6-404c-9615-dc425f67efae?collection=research