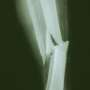
Opioids and antidepressants linked to higher fracture risk in rheumatoid arthritis patients
Opioids and selective serotonin reuptake inhibitors, a widely used group of antidepressants, are both associated with higher risk of osteoporotic fractures for patients with rheumatoid arthritis, according to new research findings presented this week at the 2017 ACR/ARHP Annual Meeting in San Diego.
Rheumatoid arthritis (RA) is a chronic disease that causes pain, stiffness, swelling, and limitation in the motion and function of multiple joints. Though joints are the principal body parts affected by RA, inflammation can develop in other organs as well. An estimated 1.3 million Americans have RA, and the disease typically affects women twice as often as men.
Chronic inflammation and pain predispose RA patients to several comorbidities including cardiovascular, mental, and gastrointestinal disorders that lead to the frequent use of multiple medications. Some of these medications have been reported to influence fracture risk in the general population, but these associations had not been studied in RA patients. Researchers at the University of Nebraska Medical Center in Omaha and the National Data Bank for Rheumatic Diseases in Wichita, Kansas, conducted a study to look at associations of various medications commonly used by RA patients with osteoporotic (OP) fracture risk.
"Even at younger ages, RA is associated with a twofold increased risk of osteoporosis and fractures due to chronic inflammation and glucocorticoid use. More importantly, osteoporotic fractures significantly contribute to the disability, health-related costs and mortality with substantially higher complication in RA patients than the general population," said Gulsen Ozen, MD, Research Fellow at the University of Nebraska Medical Center in Omaha and a lead author of the study. "Given the burden of osteoporotic fractures and the suboptimal osteoporosis care, it's highly important to identify factors associated with fracture risk, particularly modifiable ones, in RA patients."
In an observational cohort of RA patients located across the United States, the researchers studied associations between osteoporotic fracture risk and the following medications: disease-modifying antirheumatic drugs (DMARDs), statins, antidepressants (including selective serotonin reuptake inhibitors (SSRIs) and others), proton pump inhibitors (PPI), nonsteroidal anti-inflammatory drugs (NSAIDs), anticonvulsants and antipsychotics. DMARDs were categorized into four groups: methotrexate monotherapy (comparator group), TNF-inhibitors, non-TNF biologics and others, along with a separate glucocorticoid variable. All the other therapies were evaluated separately as either current use versus nonuse and also as short-term (30 days or less) or long-term (1-3 months and 3 months or more) use. The researchers also made adjustments in their analysis for socio-demographics, comorbidities, body-mass index, fracture risk according to FRAX scores and RA severity measures.
Patients from the National Data Bank for Rheumatic Diseases who were selected for the study were 40 years of age or older, and had not had a prior OP fracture from 2001-2016. They were assessed for osteoporotic fractures. The study evaluated 11,049 RA patients. During a median follow-up time of 5.7 years, the researchers found 863 osteoporotic fractures. Patients who developed fractures were significantly older and had higher disease activity, longer disease duration, higher rates of glucocorticoid use, higher fracture risk and more comorbidity at the baseline than those patients who did not experience fractures. Data in this ongoing study has been updated since the abstract was accepted.
The researchers also found significant increases in osteoporotic fracture risk when patients used SSRIs or opioids of any strength. Patients had an increase in their fracture risk starting after just one to 30 days of using opioids. Fracture risk associated with SSRI use started to rise after three months of taking these antidepressants, and the risk was more prominent with long-term use, the study showed. The increased fracture risk linked to use of opioids or SSRIs may be due to an increased risk of falls associated with these medications, the researchers concluded.
"Knowing the risks associated with the use of these medications can guide rheumatologists and other physicians in choosing the most appropriate management strategies in patients, particularly the ones who have a high fracture or fall risk," said Dr. Ozen. "Some medications have important health impacts, and it's impossible to avoid using them. In these situations, it is important that physicians are aware of the fracture risk to apply appropriate screening and preventive measures for osteoporotic fractures. Additionally, careful and regular reviewing of patient medications is an essential part of the RA patient care, as the use of medications that are not indicated anymore brings harm rather than a benefit."