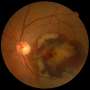
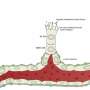
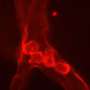
Scientists emulate the human blood-retinal barrier on a microfluidic chip
For some years, scientists have been seeking ways to reduce animal testing and accelerate clinical trials. In vitro assays with living cells are an alternative, but have limitations, as the interconnection and interaction between cells cannot be easily reproduced.
To overcome that, scientists are developing systems that mimic tissues and organ functions in conditions very close to reality. These so-called "organ-on-chip" devices include microenvironments and microarchitectures that emulate living organs and tissues.
Now, a team of scientists in Barcelona has developed a microfluidic device that mimics the human blood-retinal barrier. The scientists are from the Spanisch Council for Scientific Research (CSIC), the CIBER-BBN, and from the Institute of Health Carlos III, and the Universitat Autònoma de Barcelona (UAB). Their study, published in Lab-on-a chip, is a proof of concept that demonstrates the feasibility of the design.
Emulating the structure of the blood-retinal barrier
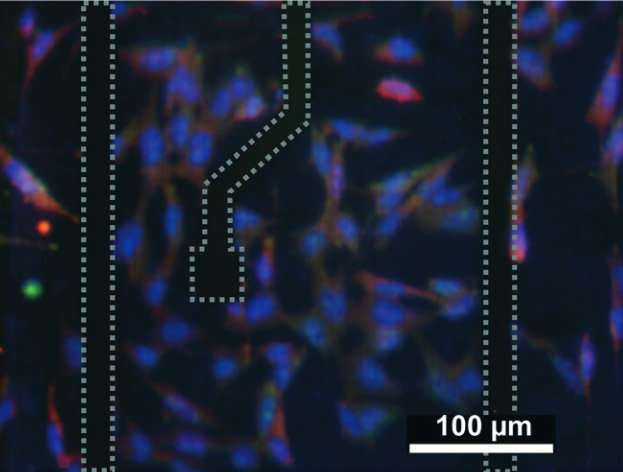
José Yeste, the main author of the study, explains that the device is composed of several parallel compartments arranged to emulate the retinal layer structure. In every compartment, a type of cell has been cultured—endothelial cells, which constitute capillary vessels which carry oxygen and nutrients; neuronal cells, which form the neuroretina; and retinal pigmented epithelial cells, which form the outer layer of the blood-retinal barrier.
The compartments are interconnected by a grid of microgrooves below, with which cells can exchange signal molecules and therefore communicate. As a result, substances produced by some cells can reach the other cells, generating cellular communication and interaction as in a living organ. Also, the device exposes endothelial cells to particular mechanical conditions that are similar the ones induced by the blood stream.

Rosa Villa, a leader of the Biomedical Applications Group, explains, "In the living organism, endothelial cells that cover the inner walls of blood vessels are exposed to the mechanical stimulus of the blood stream. In the cell cultures where this condition is not reproduced, the cells are 'sleepy,' and do not react as they would do in real conditions."
Rafael Simó, who leads the Diabetes and Metabolism group of the Vall d"Hebron Research Institute (VHIR), says, "The most relevant characteristic of this technology is that mimics what happens 'in vivo' in the retina and therefore can be an essential tool to boost the in vitro experimentation. On the device, the cells grow in contact with a fluid, as happens in the human retina. Also, the cells have a close interaction via chemical mediators, which makes it possible to see what happens in a type of cell when another type of cell nearby is harmed. Also, it is possible to measure electrical resistance for assessing the functionality of the retinal neurons."
The scientists tested the correct formation of the blood-retinal barrier assessing its permeability, its electrical resistance and the expression of some proteins of the tight junctions between cells, which are expressed when cells have established a barrier function.
The tests have been designed to check whether the barrier was properly formed, but keeping the natural permeability to allow the pass of nutrients and oxygen, and to find out if the cells were in contact and interacting. This device, the scientists say, can be used to study the effects of molecules or harmful conditions on the human retina. The team also wants to use the device to study the diabetic retinopathy, a disease whose causes and progression are not well understood yet.
Previously, the team lead by Rosa Villa at the Microelectronics Institute of Barcelona (IMB-CNM) of the CSIC created a device that emulates the blood-brain barrier. Also, they developed a liver-on-a chip microfluidic chamber that mimics the hepatic microcirculation.
More information: Jose Yeste et al, A compartmentalized microfluidic chip with crisscross microgrooves and electrophysiological electrodes for modeling the blood–retinal barrier, Lab on a Chip (2017). DOI: 10.1039/C7LC00795G