Research is changing the game for melanoma treatment
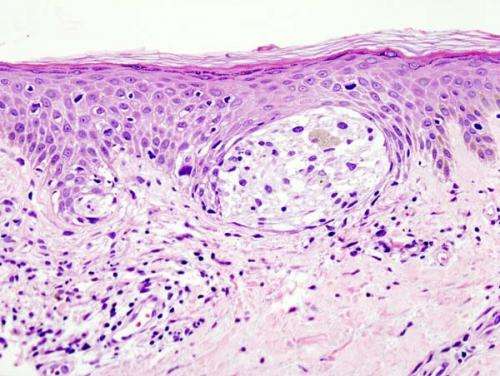
Wilmot Cancer Institute patients with advanced melanoma (stage III) now have more options for treatment, thanks to research co-authored by a University of Rochester Medical Center surgical oncologist and published in The Lancet Oncology.
The study involved comparing two treatment approaches for high-risk melanoma patients with a BRAF gene mutation in their cancer: standard care, which calls for upfront surgery, or giving a two-drug, targeted therapy regimen before surgery and again afterward. Patients in the latter group had longer disease-free survival in the Phase 2 trial, and after seven months researchers halted the study earlier than expected due to the positive results.
"What's so exciting is that neoadjuvant therapy (giving a cancer drug before surgery) had never been done before in melanoma," said Peter Prieto, M.D., M.P.H., assistant professor of Surgery and Oncology at URMC, who helped to lead the study when he was completing a fellowship at MD Anderson Cancer Center. He joined the faculty in Rochester last year.
"And in this trial we not only saw that patients receiving the neoadjuvant therapy were doing much better, but 58% of them had a complete pathologic response. That means that when their tumor was removed it had no viable cancer cells in it," Prieto said.
Eligible Wilmot patients would have a surgically removable stage III or stage IV melanoma with a mutation of the BRAF gene. (Many cancers in this category are in the process of transitioning from localized disease to becoming widespread, defined as oligometastatic cancer.) Currently less than 50 percent of individuals in this high-risk category are alive, five years after diagnosis. But now, in most cases, they will be able to receive the new treatment approach, Prieto said.
Having a BRAF gene mutation is a key ingredient to this treatment. During the last decade researchers have been able to transform care of melanoma skin cancer because of the development of drugs that target the gene defect. Approximately 60 percent of melanomas have the mutation, and targeting the BRAF gene with medication works in 90 percent of these cases, Prieto said.
Most clinical studies targeting the BRAF mutation began in patients who had stage IV cancer (the disease had already spread to other organs or parts of the body). Now, Prieto said, with the knowledge of how to treat stage 4 patients, doctors and scientists can apply the same principles to earlier-stage melanoma.
The published study was a small, randomized trial, enrolling 21 patients before it was stopped. The group of patients in the arm that showed longer survival received two drugs (dabrafenib and trametinib) for eight weeks prior to surgery, underwent surgery, and then continued to take the two-drug combination after surgery for 44 more weeks. The most common side effects were chills and headache.
Prieto said it is still unclear how many weeks the drug should be given to patients after surgery. Researchers are continuing to look into that question; his lab at URMC is also investigating how to predict which patients are most likely to land in the "complete pathologic response" category if they receive the regimen.
The concept of pre-treating malignant tumors prior to surgery is on the rise for many different types of cancers as researchers identify more gene mutations that can be precisely targeted with newer drugs.
More information: Rodabe N Amaria et al. Neoadjuvant plus adjuvant dabrafenib and trametinib versus standard of care in patients with high-risk, surgically resectable melanoma: a single-centre, open-label, randomised, phase 2 trial, The Lancet Oncology (2018). DOI: 10.1016/S1470-2045(18)30015-9













