Researchers discover a potential new therapeutic strategy for pancreatic cancer
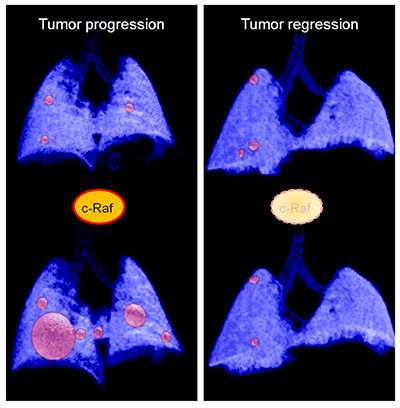
In most pancreatic cancer patients, the diagnosis occurs when the disease is already advanced, and currently, there is no effective treatment. There have been no significant advances to combat it in recent decades, and unfortunately, its occurrence is on the increase. Now, a group of researchers from the Spanish National Cancer Research Centre (CNIO) may have found a new therapeutic approach. The research is published in the Proceedings of the National Academy of Science (PNAS).
One of the characteristics of pancreatic cancer is that the tumour cells are embedded in the stroma, which represents 90 percent of the tumour mass and which seems to form a barrier (physical and chemical) hindering treatment with inhibitors, chemotherapy and immunotherapy. Most of the studies have focused mainly on tumour cells rather than the stroma, in spite of research proving that components of the stroma promote the tumour progression. Recently, researchers have tried to eliminate the most abundant cells in the stroma, the so-called cancer associated fibroblasts (CAFs), but found that the tumours became more aggressive. The interpretation of this result was that some of the cells eliminated could have anti-tumorigenic functions.
Therefore, researchers from the CNIO's Experimental Oncology Group have focused their work on identifying a stromal cell population that fosters tumour growth, to later discover why they have this capacity and reverse it. The strategy to achieve the latter is innovative, because instead of eliminating these stromal cells which help the tumour, the objective has been their selective reprogramming.
As Carmen Guerra, one of the lead researchers, and Magdolna Djurec, first author of the work, explain "there are now many groups looking into the relationship of the stroma and tumour growth, with the hope of finding new therapeutic strategies. We have seen that eliminating stromal cells may have a negative effect, so our approach is to reprogramme the stroma instead of eliminating it. It is an innovative strategy."
The researchers focused on a subpopulation of fibroblasts known to play a role in inflammation, because inflammation fosters tumour growth. Their first task was to analyse all of the genes that are differentially expressed in the stromal fibroblasts of the tumour, the CAFs, in comparison with the fibroblasts of healthy pancreatic tissue. Their hypothesis was that the possible genes responsible for the pro-tumour role of the CAFs would be expressed at high levels only in these fibroblasts, and not in fibroblasts of the healthy tissue.
The analysis revealed that the Saa3 gene is responsible for CAFs helping tumour cells to progress. When the researchers eliminated the expression of this gene in the CAFs, these cells behaved like normal fibroblasts, losing the ability to accelerate tumour cell progression. Researchers had managed to "reprogramme" these cells, which had been stripped of their pro-tumour properties.
"This finding may represent a future therapeutic strategic to combine with other strategies, such as immunotherapy, chemotherapy or inhibitors against specific signalling routes of the tumour cells. It opens the door to new research in many laboratories aimed at reprogramming the stroma instead of eliminating it," added Djurec.
It is still too early to think about its clinical application, but the work reveals a new genetic target for possible therapeutic strategies. In human samples of pancreatic cancer, the researchers have identified the same population of pro-tumour fibroblasts, and have observed that when the SAA1 gene (the human version of Saa3) is overexpressed, the prognosis for the patients is far worse. The researchers are still studying the role of other potentially relevant genes found in the comparative expression analysis of the CAFs and normal fibroblasts.
More information: Magdolna Djurec et al, Saa3 is a key mediator of the protumorigenic properties of cancer-associated fibroblasts in pancreatic tumors, Proceedings of the National Academy of Sciences (2018). DOI: 10.1073/pnas.1717802115