Recreating liver tumors as organoids for faster, more accurate drug screening
Liver cancer is one of the top causes of cancer deaths globally, with a lack of approved treatments. A major challenge in developing effective drugs for liver cancer is that current preclinical tumor models do not accurately replicate features of the tumor and the tumor environment in humans, causing many potential drugs to fail in clinical testing.
To more accurately mimic these features, researchers have developed models of liver tumors called patient-derived xenografts (PDX). Although these models provide a truer picture of how effective potential cancer drugs would be in humans, they are also expensive and time-consuming to create. Growing these PDX cancer cells in culture would be more cost effective for drug screening. However, current attempts to culture these cells fail to reflect the 3-D tumor structure and the tumor environment.
Led by Dr. Eliza Fong and Dr. Toh Tan Boon, an interdisciplinary team of researchers at the NUS Departments of Physiology and Biomedical Engineering, the Cancer Science Institute of Singapore, the Institute of Bioengineering and Nanotechnology, A*STAR and the National Cancer Center Singapore has now devised a new method to grow PDX liver cancer cells for use in drug testing.
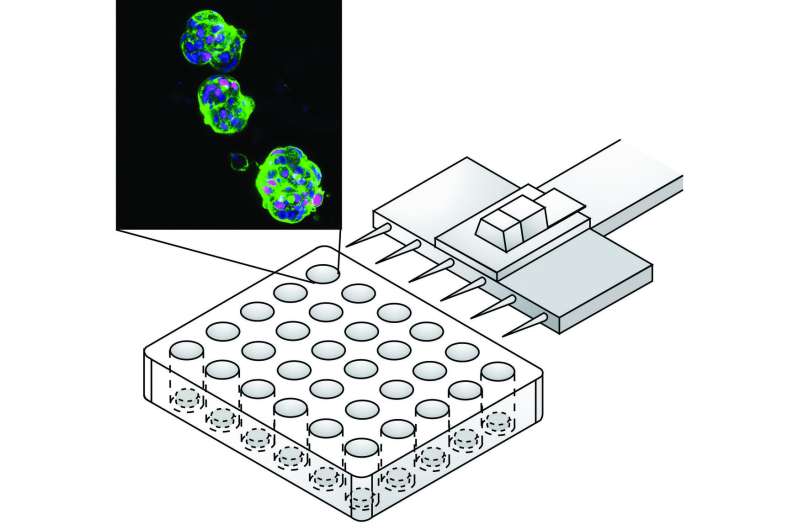
As described in their recent paper in Biomaterials, this method involves growing the cells on synthetic 3-D scaffolds made of a plant-based porous hydrogel. The researchers engineered the spongy scaffolds with optimized biochemical and mechanical properties to help the liver cancer cells maintain their proper shape and function and grow as organoids.
After growing the organoids for one to three weeks, the team verified that the liver cancer cells in the organoids were alive and reproducing. Liver cancer cells usually contain specific genetic changes that are absent in normal liver cells. The researchers engineered organoids from PDX that were taken from 14 liver cancer patients. Most of the organoids retained the same key genetic changes that were in the source PDX cells. They also maintained an important feature of liver tumors called intra-tumor heterogeneity, in which distinct populations of liver cancer cells are present within the same tumor and affect its response to treatment. The presence of this feature was another advantage for drug screening that the organoids have over traditional cell culture methods, in which all cells are identical.
As a bioengineer, Dr. Fong finds the success of the engineered organoids to be particularly rewarding. "This study truly epitomizes the positive synergy we can achieve in growing patient tumors outside the body by marrying advances in tissue engineering with cancer biology," she says.
Another attractive feature is the small size of the 3-D scaffolds containing the organoids—a mere 100 microns. They can easily fit inside the well of a 96-well microtiter plate, a standard platform for high-throughput drug screening, which enables testing many drugs at the same time. Through this technology, one PDX can be used to produce tens to hundreds of such organoid-containing scaffolds. Combined with their ability to recapitulate the genetic features and heterogeneity of the original liver tumors, these tumor avatars have the potential to revolutionize the screening and development of liver cancer drugs.
Dr. Toh says, "Having a reliable platform to grow liver cancer patient-derived cells is a major step in personalized medicine as we can now use them for increased throughput drug sensitivity testing."
Dr. Hanry Yu, Professor of Physiology at NUS Medicine, says, "The spongy scaffolds developed to keep normal liver cells happy also preserve the important properties of liver cancer for drug testing. This allows patients to choose the best treatment based on the drug testing results on their own liver cancer cells."
More information: Eliza Li Shan Fong et al, Generation of matched patient-derived xenograft in vitro-in vivo models using 3D macroporous hydrogels for the study of liver cancer, Biomaterials (2018). DOI: 10.1016/j.biomaterials.2017.12.026