An international study is the first large survey on epilepsy
An international research consortium used neuroimaging techniques to analyze the brains of more than 3,800 volunteers in different countries. It's the largest study of its kind ever conducted, and set out to investigate anatomical similarities and differences in the brains of individuals with different types of epilepsy and to seek markers that could help with prognosis and treatment.
Seizure frequency and severity, as well as the patient's response to drug therapy, vary with the part of the brain affected and other poorly understood factors. Data from the scientific literature suggests that roughly one-third of patients do not respond well to anti-epileptic drugs. Research has shown that these individuals are more likely to develop cognitive and behavioral impairments over the years.
The new study investigated several neurological and psychiatric diseases. Twenty-four cross-sectional samples from 14 countries were included in the epilepsy study. Altogether, the study included data for 2,149 people with epilepsy and 1,727 healthy control subjects (with no neurological or psychiatric disorders). The Brazilian Research Institute for Neuroscience and Neurotechnology (BRAINN) recruited the largest sample, 291 patients and 398 controls.
"Each center was responsible for collecting and analyzing data on its own patients. All the material was then sent to the University of Southern California's Imaging Genetics Center in the US, which consolidated the results and performed a meta-analysis," said Fernando Cendes, a professor at UNICAMP and coordinator of BRAINN.
All volunteers were subjected to MRI scans. According to Cendes, a specific protocol was used to acquire three-dimensional images. "This permitted image post-processing with the aid of computer software, which segmented the images into thousands of anatomical points for individual assessment and comparison," he said.
Advances in neuroimaging techniques have enabled the detection of structural alterations in the brains of people with epilepsy that hadn't been noticed previously. Cendes said that this is the first epilepsy study built on a really large number of patients, which allowed researchers to obtain more robust data. "There were many discrepancies in earlier studies, which comprised a few dozen or hundred volunteers."
The patients included in the study were divided into four subgroups: mesial temporal lobe epilepsy (MTLE) with left hippocampal sclerosis, MTLE with right hippocampal sclerosis, idiopathic (genetic) generalized epilepsy, and a fourth group comprising less-common subtypes of the disease.
The analysis covered patients who had epilepsy for years, and patients who had been diagnosed recently. According to Cendes, the analysis aimed at the identification of atrophied brain regions in which the cortical thickness was smaller than in the control group. The results were published in Brain.
First analysis
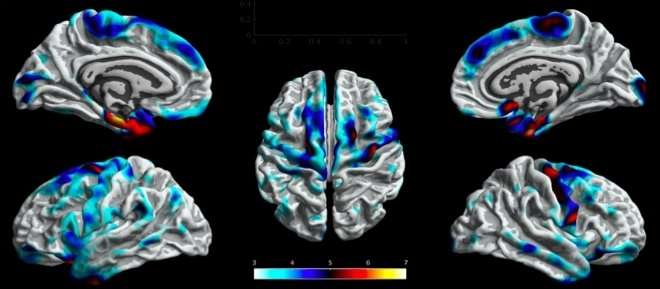
The researchers first analyzed data from the four patient subgroups as a whole and compared them with the controls to determine whether there were anatomical alterations common to all forms of epilepsy. "We found that all four subgroups displayed atrophy in areas of the sensitive-motor cortex and also in some parts of the frontal lobe," Cendes said.
"Ordinary MRI scans don't show anatomical alterations in cases of genetic generalized epilepsy," Cendes said. "One of the goals of this study was to confirm whether areas of atrophy also occur in these patients. We found that they do."
This finding, he added, shows that in the case of MTLE, there are alterations in regions other than those in which seizures are produced (the hippocampus, parahippocampus, and amygdala). Brain impairment is, therefore, more extensive than previously thought.
Cendes also noted that a larger proportion of the brain was compromised in patients who had had the disease for longer. "This reinforces the hypothesis that more brain regions atrophy and more cognitive impairment occurs as the disease progresses."
The next step was a separate analysis of each patient subgroup in search of alterations that characterize each form of the disease. The findings confirmed, for example, that MTLE with left hippocampal sclerosis is associated with alterations in different neuronal circuits from those associated with MTLE with right hippocampal sclerosis. "Temporal lobe epilepsy occurs in a specific brain region and is therefore termed a focal form of the disease. It's also the most common treatment-refractory subtype of epilepsy in adults," Cendes said. "We know it has different and more severe effects when it involves the left hemisphere than the right. They're different diseases."
"These two forms of the disease are not mere mirror-images of each other," he said. "When the left hemisphere is involved, the seizures are more intense and diffuse. It used to be thought that this happened because the left hemisphere is dominant for language, but this doesn't appear to be the only reason. Somehow, it's more vulnerable than the right hemisphere."
In the GGE group, the researchers observed atrophy in the thalamus, a central deep-lying brain region above the hypothalamus, and in the motor cortex. "These are subtle alterations but were observed in patients with epilepsy and not in the controls," Cendes said.
Genetic generalized epilepsies (GGEs) may involve all brain regions but can usually be controlled by drugs and are less damaging to patients.
From his vantage point, the findings published in the article will benefit research on the subject, and have implications for the future diagnosis of the disease. In parallel with their anatomical analysis, the group is also evaluating genetic alterations that may explain certain hereditary patterns in brain atrophy. The results of this genetic analysis will be published soon.
"If we know there are more or less specific signatures of the different epileptic subtypes, instead of looking for alterations everywhere in the brain, we can focus on suspect regions, reducing cost, saving time and bolstering the statistical power of the analysis. Next, we'll be able to correlate these alterations with cognitive and behavioral dysfunction," Cendes said.
More information: Christopher D Whelan et al, Structural brain abnormalities in the common epilepsies assessed in a worldwide ENIGMA study, Brain (2017). DOI: 10.1093/brain/awx341