Humira does not improve aortic vascular inflammation in psoriasis patients
An antibody used to treat the skin disease psoriasis and other chronic autoimmune diseases such as rheumatoid arthritis and inflammatory bowel disease has no effect on aortic inflammation—a key marker of future risk of major cardiovascular events—unlike other antibodies that target different aspects of the immune system. Researchers from the Perelman School of Medicine at the University of Pennsylvania, in collaboration with the National Heart, Lung, and Blood Institute (NHLBI), led a multi-center, randomized, double-blind, placebo-controlled study and found patients taking the drug adalimumab—marketed as Humira—saw no change in aortic inflammation, as assessed by nuclear imaging, when compared to the placebo group. However, the drug did improve other key markers of inflammation known to predict future cardiovascular events—which suggests the drug may have a cardiovascular benefit despite the lack of change in aortic vascular inflammation. The study was published today in the journal Circulation: Cardiovascular Imaging, and senior author Joel M. Gelfand, MD MSCE, a professor of Dermatology and Epidemiology at Penn, will present the findings today at the International Investigative Dermatology 2018 Annual Meeting in Orlando, Florida.
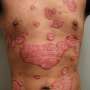
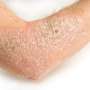
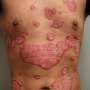
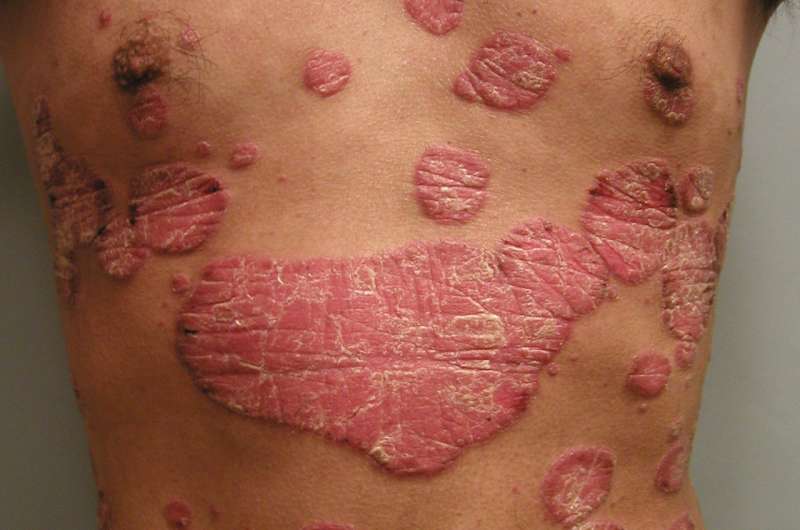
Psoriasis is a chronic inflammatory disease that causes skin cells to multiply faster than normal resulting in raised, red patches covered by silvery scales. It occurs most commonly on the scalp, knees, and elbows but can appear anywhere on the body including the face, genitals, nails, and other places. In moderate to severe cases, it carries an increased risk of heart attack, stroke, and premature death, a finding established by Gelfand in a 2006 landmark study. The National Psoriasis Foundation estimates psoriasis affects about 7.5 million Americans.
Adalimumab is an antibody that blocks tumor necrosis factor alpha (TNF-a), a protein that promotes inflammation in the body. It's approved by the U.S. Food and Drug Administration to treat psoriasis, psoriatic arthritis, rheumatoid arthritis, ulcerative colitis, and Crohn's Disease, among other conditions. TNF inhibitors are the most popular prescribed biologic medications for inflammatory diseases, and Penn researchers have previously found another biologic drug, ustekinumab (Stelara), led to a 19 percent reduction in aortic inflammation in psoriasis patients. The researchers wanted to know whether adalimumab provided a similar benefit.
Ninety-seven patients at eight different enrollment sites were randomly divided into three groups. One group received adalimumab, another received a placebo, and a third received Ultraviolet B phototherapy—another common treatment for psoriasis which works by suppressing inflammation locally in the skin as opposed to systemically, as is the case with adalimumab. Patients were evaluated at 12 weeks, and patients in the two active treatment groups saw significant improvement in their psoriasis relative to placebo. At the end of the initial 12 weeks, all patients received adalimumab—with those already on the drug getting 40 weeks and those taking it for the first time getting 52 weeks so all patients ended up with 52 weeks of treatment.
At both the 12-week and 52-week evaluation periods, patients in the adalimumab group saw no change compared to placebo or baseline, respectively, in aortic vascular inflammation. Patients receiving phototherapy saw a four percent reduction compared to baseline at 12 weeks but the difference was not statistically significant from placebo.
"These results are similar to prior clinical trials which showed adalimumab did not reduce aortic inflammation in patients with psoriasis. They are, however, in contrast to a previous study which showed an improvement in aortic vascular inflammation at 12 weeks in patients taking ustekinumab—a biologic that targets a different aspect of the immune system," Gelfand said.
Despite neutral imaging results, adalimumab did improve other key markers of inflammation in the blood including GlycA, CRP, TNF, and IL-6.
"Each of these increases future risk of heart attack and diabetes, so observing a reduction of these markers of systemic inflammation provides compelling evidence of beneficial effects of anti-TNF therapy in psoriasis," said the study's lead author Nehal N. Mehta, MD MSCE FAHA, chief of the Laboratory of Inflammation and Cardiometabolic Diseases at the NHLBI.
Understanding cholesterol effects of adalimumab by new techniques was another goal of Gelfand and Mehta's study.
"We know that HDL, the good cholesterol, is low in psoriasis, but here, we now show that despite reduction in systemic inflammation following adalimumab therapy, HDL particle size got smaller (not a good thing) and the HDL worked less effectively to remove cholesterol from the body," Mehta said.
Gelfand noted the impact on HDL may be balanced by the improvement seen in markers of systemic inflammation that are reduced as psoriasis improves. Gelfand also emphasized that this class of drug is commonly used, so understanding its potential cardiovascular effects is highly important. Future studies in this area are already underway at Penn and the NHLBI.