The influence of circadian rhythms on atherosclerosis
The internal clock controls all vital functions in the body. Body temperature as well as blood pressure or the release of certain enzymes are subject to oscillations throughout the day, the so-called circadian rhythm. For the first time, a team around Professor Oliver Söhnlein has now shown the influence of circadian rhythms on atherosclerosis—a vascular disease that ultimately can lead to heart attacks and strokes. His study, recently published in the scientific journal Cell Metabolism, could be crucial for the improvement of therapeutic approaches.
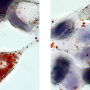
Oliver Söhnlein researches molecular mechanisms underlying atherosclerosis at the Institute for Cardiovascular Prevention. During this disease, lipid deposits can form on the inner vascular wall of large arteries. Cells of the immune system travel from the blood to the damaged location and attract more and more cells via signaling substances until the immune reaction finally derails. Atherosclerotic inflammation develops over years; however, the recruitment of cells is subject to circadian rhythms as Söhnlein has proven in mouse models of atherosclerosis. "At certain times of the day, three times as many leukocytes travel to the center of arterial inflammation as it is the case for other times," says Söhnlein. This rhythmic migration pattern is about 12 hours phase shifted with the recruitment pattern observed in the microcirculation in small veins.
Precisely this shift between the two vascular systems is interesting from a therapeutic aspect. "The recruitment of white blood cells in the micro-circulation is important for acute infections such as for example a lung or bladder infection," explains Oliver Söhnlein. Ideally, the recruitment of immune cells is to be stopped for the atherosclerotic inflammation but not in the micro-circulation.
The researchers of LMU achieved just that with their work in an early stage of atherosclerosis: On the one hand, they identified the molecular mechanism how rhythmic arterial leukocyte migration is controlled. On the other hand, timed inhibition of this pathway centered on the chemokine CCL2, they were able to stop the recruitment only into atherosclerotic areas but did not affect microvascular leukocyte migration. "Our study shows how circadian patterns can be used for timed therapeutic intervention possibly with lower side effects and higher efficacy," says Söhnlein.
In further studies the researchers want to examine to which extent circadian rhythms contribute to destabilization for advanced atherosclerosis. In addition, they want to focus on studying the circadian regulation of processes in the atherosclerotic deposits themselves, for example the question whether cell death is controlled in a circadian fashion.