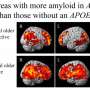
Advances along the gut-liver-brain axis in Alzheimer's disease
Four new studies reported at the Alzheimer's Association International Conference (AAIC) 2018 in Chicago investigated how the digestive system, including gut and liver functions, may be related to changes in the brain, and to brain disorders such as Alzheimer's disease and other dementias.
The gut microbiome is the community of microorganisms that live in the digestive tracts of humans and other animals—about a thousand different species of bacteria, comprising trillions of cells. Emerging science has correlated certain changes in the gut bacteria with a variety of inflammatory and autoimmune conditions. And studies have shown that changes in diet can change the gut bacteria.
In research reports over the last few years, we've learned a great deal about how diet, particularly overall eating patterns, may be linked to brain health, cognitive decline and possibly even dementia as we age. We've also seen inflammation and its markers—in the brain and other parts of the body—associated with Alzheimer's and other dementias.
Exactly how diet and gut microbes interact with the brain, and influence the brain's health—as a cause, trigger or risk/protective factor—is a relatively new area of investigation for Alzheimer's and other dementias. For example, recently, scientists have reported that some species in the microbiome can promote protein buildup in the brain. This may be significant because accumulation of amyloid and tau proteins are hallmarks of Alzheimer's disease. And recent reports from experiments in mouse models engineered to have Alzheimer's-like changes and symptoms suggest that changing the bacterial profile in their digestive tract—by changing their diet—may reduce amyloid plaques, lower inflammation and improve memory.
At the same time, an increasing body of evidence suggests that altered metabolism of certain lipids may be an important factor in the development of Alzheimer's. Several of the genes associated with Alzheimer's—including the strongest Alzheimer's risk gene, APOE-e4—are involved in lipid transport or metabolism. In addition, lipids make up most of the brain's mass, so changes in the production or transport of lipids may have a significant effect on brain structure and function. Key functions of lipids include storing energy and acting as structural components of cell membranes.
"While still in its infancy, gut microbiome research is very exciting since it may give us a new window into why diet and nutrition are so important for brain health," said Maria Carrillo, Ph.D., Alzheimer's Association Chief Science Officer. "For example, this work may tell us more about how and why 'good fats' help keep the brain healthy, and help guide brain-healthy dietary choices."
"In addition, if it turns out these gut bacteria are effective and accurate markers of Alzheimer's disease cause or progression, or both, they might be useful as a non-invasive screening tool—a simple blood test. They could then be used to help identify high-risk people for clinical trials or track the impact of a therapy," Carrillo said. "However, we are only at step one. We don't know yet exactly what the changes we are seeing mean—especially in animal models—whether they are cause or effect."
Does the Liver Contribute to Alzheimer's Risk by Failing to Supply Key Lipids to the Brain?
Researchers of the Alzheimer's Disease Metabolics Consortium (ADMC), led by Rima Kaddurah-Daouk, Ph.D., Professor of Psychiatry at Duke University who leads the ADMC, and in this study by Mitchel A. Kling, MD, Associate Professor of Psychiatry in the Perelman School of Medicine at the University of Pennsylvania, found that reduced levels of plasmalogens, a class of lipids that are integral to cell membranes, were associated with an increased risk of Alzheimer's. Data also suggested statistically-significant differences in plasmalogen metabolism between Alzheimer's and comparison groups, and that some of the plasmalogen levels were correlated with cerebrospinal fluid (CSF) levels of total tau protein.
Plasmalogens synthesized in the liver are taken up by many types of tissues, including the brain. The most abundant plasmalogens contain the omega-3 fatty acids docosahexaenoic acid (DHA) and eicosapentaenoic acid (EPA), which have received research interest due to their potential anti-inflammatory properties. However, previous studies have failed to convincingly demonstrate a beneficial effect of these substances in people with Alzheimer's.
The researchers measured several plasmalogens, including those containing DHA and EPA, as well as those containing the omega-6 fatty acid adrenic acid and closely-related lipids, in stored blood-based fluids collected from two groups:
- 304 subjects with Alzheimer's, 876 with mild cognitive impairment (MCI) or significant memory concerns (SMC), and 367 who were cognitively normal (CN), enrolled in the Alzheimer's Disease Neuroimaging Initiative (ADNI)-1, -GO, or -2 studies; and
- 112 subjects including 43 with Alzheimer's, 18 with MCI, and 51 CN enrolled at the Penn Memory Center at the Perelman School of Medicine, University of Pennsylvania.
"The data suggest that reduced production of plasmalogens by the liver may result in reduced availability of these critical lipids to the brain. This may contribute to impaired cognitive function and neurodegeneration in Alzheimer's," Kling said. "These data provide a possible explanation for the lack of effect of fish oil or DHA on cognitive function or Alzheimer's in previous studies."
The researchers, who are part of the M2OVE-AD consortium, funded by the U.S. National Institute on Aging (NIA), are currently trying to better understand the connection between altered liver and brain function in Alzheimer's, and possibly identify new targets for treatment and prevention.
"New data is emerging on the role of billions of bacteria that live within us and affect our health through the chemicals they produce—some are beneficial while others lead to disease," said Kaddurah-Daouk. "The gut microbiome has been implicated in diseases like Parkinson's, autism and depression, and only recently have we started to focus on its possible role in Alzheimer's disease—looking at possible links between gut bacteria, cognitive changes and brain changes."
Altered Bile Acid Metabolites in MCI and Alzheimer's: Relation to Neuroimaging and CSF Biomarkers
To date, relatively little research has been done in humans to link peripheral metabolic changes in cholesterol to biomarkers related to Alzheimer's, including amyloid and tau accumulation, brain glucose metabolism, and structural atrophy.
As reported at AAIC 2018, ADMC researchers measured serum levels of 15 bile acid metabolites and their eight ratios from older adults with early stage Alzheimer's or who were at risk for the disease from the Alzheimer's Disease Neuroimaging Initiative (ADNI) cohort. They assessed the association of bile acids with the amyloid, tau, and neurodegeneration biomarkers for Alzheimer's based on the recently proposed National Institute on Aging-Alzheimer's Association 2018 Research Framework using cerebrospinal fluid (CSF) and neuroimaging biomarkers (brain atrophy measured by MRI, and brain glucose metabolism measured by FDG-PET).
Primary bile acids are those synthesized from cholesterol in the liver. The main function of bile acids is to allow digestion of dietary fats and oils, including cholesterol. They also have hormonal actions throughout the body.
The scientists, supported by the NIA-led Accelerating Medicines Partnership-Alzheimer's Disease (AMP-AD) program, found an association between markers of the gut microbiome and liver function and Alzheimer's-related structural and functional neuroimaging biomarkers, and also with biomarkers of CSF amyloid-β and tau burden. In this study population, gut microbiome-produced bile acids are increased in people with Alzheimer's and are associated with functional and structural brain changes including cognitive decline, reduced brain glucose metabolism, and greater brain atrophy. Further, these same bile acids were associated with increased amyloid and tau accumulation. For example:
- Lower serum concentrations of one primary bile acid (CA) were significantly associated with worse cognition, decreased hippocampal volume and decreased brain glucose metabolism.
- Higher serum concentrations of one conjugated primary bile acid (GCDCA) and two bacterially-produced conjugated secondary bile acids (GLCA and TLCA) were significantly associated with higher CSF p-tau and CSF t-tau values, decreased hippocampal volume and decreased brain glucose metabolism.
- Higher serum concentrations of three ratios of bacterially-produced conjugated secondary bile acids to primary bile acids (TDCA:CA, GDCA:CA, and GLCA:CDCA) were associated with lower CSF Aβ1-42 values, decreased hippocampal volume and decreased brain glucose metabolism.
"We believe this is the first study to show that serum-based altered (higher or lower) bile acid profiles are associated with amyloid, tau, and neurodegeneration biomarkers of Alzheimer's disease," said Kwangsik Nho, Ph.D., Assistant Professor of Radiology and Imaging Sciences at the Center for Neuroimaging at the Indiana University School of Medicine. "Further research is needed to assess what is causing the changes in bile acids and the specific mechanisms underlying this association."
Circulating Metabolites Associated with Alzheimer's Disease Genetic Variants
Recent studies suggest that bile acids involved in cholesterol metabolism and clearance are somehow associated with Alzheimer's disease. At the same time, large genome-wide association studies have discovered more than 25 genetic variants associated with Alzheimer's, including several that are involved in lipid metabolism. Shahzad Ahmad, MSc, a Ph.D. student at Erasmus Medical Center, Rotterdam, and colleagues evaluated if Alzheimer's genetic variants can influence the level of cholesterol, bile acids and other biochemical compounds in blood.
The researchers used 5,974 samples for analysis of subtypes of cholesterol (known as sub-fractions)—4,647 from the Rotterdam Study (RS) and 1,327 from the Erasmus Rucphen family study (ERF). For bile acid analysis, the dataset consisted of a separate group of 488 participants from RS.
The researchers found that genetic variations in Alzheimer's risk genes APOE-e4 and SORL1 were significantly associated with decreased levels of some of the cholesterol components that may be important for the health and repair of brain cell membranes (p<1x10-5). Alzheimer's-associated genetic variants in ABI3, TREM2, MS4A6A and ABCA7 were associated with bile acids (deoxycholate, glycodeoxycholate sulfate, and the deoxycholate to cholate ratio) and certain lipids (p<1x10-3). In addition, the team found that bile acids cluster with caffeine levels in the blood, suggesting a possibility for lifestyle interventions.
"Our hope is that, once validated, these associations between the genome and metabolome in Alzheimer's will reveal causal pathways," said Ahmad. "These then may become targets for therapies or prevention strategies."
Ahmad added, "The brain is connected to the rest of the body, so identifying gut microbes that change the levels of these biochemical compounds in the body is a plausible next step towards identifying new potential therapeutic approaches for Alzheimer's."
Association of Serum Lipids with Alzheimer's Disease in the ADNI Cohort
Lipids are a major component of brain membranes. It is believed that they can influence the accumulation of toxic peptides—amyloid and tau—that are related to Alzheimer's disease. Blood flow supplies lipids to the brain, and a majority of circulating lipids are synthesized in the liver and gut, which supports the idea that our body's organs can influence brain functions.
Researchers in the ADMC and UC Davis-West Coast Metabolomics Center measured the levels of more than 400 lipids in blood samples from ADNI-1, which has 200 normal, 400 mild cognitive impaired and 200 Alzheimer's participants. They evaluated the association of those lipids with Alzheimer's diagnosis, brain atrophy, amyloid and tau accumulation, and cognitive decline using a new method of clustering lipids by chemical similarity.
They found that lipid metabolism is disturbed in people with Alzheimer's in the ADNI-1 study population. Several lipids were significantly altered in people with Alzheimer's with failures in proper incorporation of unsaturated fatty acids specifically EPA, DHA (fish oils) and Arachidonic acid in these lipid classes. Obese and male subjects had the strongest disturbance. Fish oil intake by people with Alzheimer's in the study failed to bring the levels of these lipids back to normal.
"We think these results help explain the poor results of the clinical trials of fish oil trials for treatment of Alzheimer's," said Dinesh Kumar Barupal, Ph.D., a project scientist and the program coordinator for the NIH-funded West Coast Metabolomics Center at the University of California, Davis. "And they may help uncover new therapeutic strategies targeting lipid metabolic pathways and failures within the liver."