Uncovering the whole story in diabetes
More than 400 million people worldwide suffer from type 2 diabetes, a disease characterised by increased blood glucose levels, because the body's normal way of controlling insulin release breaks down.
But insulin is only one half of the story about what goes wrong in type 2 diabetes: the release of another hormone called glucagon, which has an opposite effect to insulin, is also disrupted in type 2 diabetes.
Now a study led by Professor Patrik Rorsman from the Radcliffe Department of Medicine has found that exposure to high glucose levels for as little as 48 hours changes glucagon secretion from the pancreas – but there may be a way to reverse these effects to restore normalcy.
The study, published in the journal Cell Metabolism, used mice that had been genetically altered to mimic the symptoms of type 2 diabetes, as well as cells from the pancreas' 'islets," donated by patients with type 2 diabetes.
Unique cells
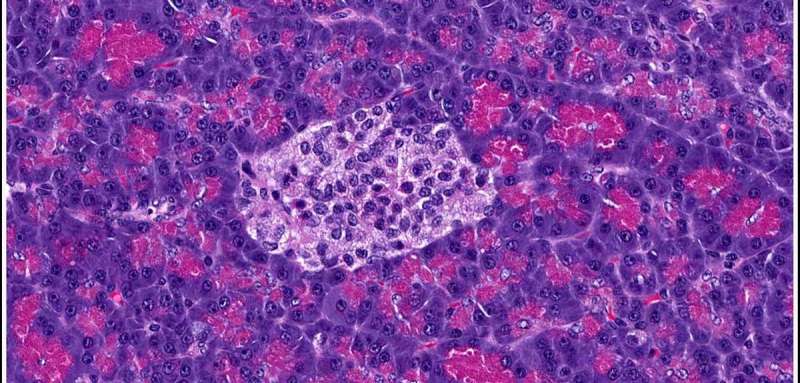
Endocrine cells, such as the alpha cells in the pancreatic islets, are excitable cells that can generate electrical pulses (known as action potentials), much like cells in the brain. Alpha cells and other pancreatic islet cells use these electrical signals to control the release of islet hormones (which include both insulin and glucagon). By studying the electrical behaviour of the alpha cells, Professor Rorsman's research group (based at the Oxford Centre for Diabetes, Endocrinology and Medicine) hopes to understand how glucagon secretion is regulated.
"We actually use electrophysiology methods similar to those used by neuroscientists to record from these cells," said Dr. Quan Zhang, one of the study co-authors.
"There are only about 1g of pancreatic islets in the body and only 10% of these are alpha cells, so it's quite a painstaking process to find and study them," said Professor Rorsman. "Our group has really specialised in studying these cells, and we've probably studied more of these cells than any other group in the world!"
These alpha cells release a hormone called glucagon, which helps the liver to convert its store of glycogen into glucose, which then gets released into the bloodstream. The result is more glucose in the blood.
Insulin, which is also released by the pancreas, has the opposite effect: it signals the body to absorb glucose from the bloodstream, resulting in less glucose in the blood.
Normally, high levels of glucose result in pancreatic beta cells releasing insulin, so that glucose levels go down, and low levels of glucose result in the pancreatic alpha cells releasing glucagon, so that glucose levels go up.
"But this fine balance gets entirely disrupted in type 2 diabetes," said Dr. Jakob Knudsen, the first author of the study . "In type 2 diabetes, high glucose levels instead spur pancreatic alpha cells to release even more glucagon, which just makes glucose levels spike even higher."
Blocking the cascade
But what is actually going wrong in alpha cells to produce this strange response? The research team studied this by tracking what happens to alpha cells exposed to high levels of glucose, using mice that had been bred to have changes similar to those experienced by patients with type 2 diabetes.
The team compared what happened in diabetic versus normal alpha cells, and found that exposure to high glucose levels for as little as 24 hours set off a complex cascade of cellular processes that led to more sodium being 'pushed' into the alpha cells.
This lowered the cells' pH, which results in lower energy being available to the cell. The lower energy levels change the activity of an energy sensitive channel in the cell membrane, and ultimately result in the glucagon release going awry.
But crucially, the researchers were able to reverse too much glucagon secretion in both the cells and the mice by using a drug that stopped too much sodium from getting into alpha cells, thus blocking the chain of events that led to glucagon dysregulation right at the start.
High levels of glucose leave a mark
However, high levels of glucose still left their mark: overweight diabetic rats who had bariatric weight reduction surgery (similar to humans) or successful diabetes drug treatment still had protein changes in alpha cells caused by high levels of glucose—even after their glucose levels returned to normal. What's more, these protein changes weren't restricted to the pancreas: the researchers found similar changes in heart and kidney cells in diabetic mice, even when their glucose levels had returned to normal.
"We're still understanding the complex interplay that leads to diabetes, but we're hoping that drugs that inhibit these protein changes might be one way of treating the disease," said Professor Rorsman. "Indeed, we already know that some drugs with inhibit the 'transporter' through which sodium gets into alpha cells have had a positive effect in diabetes in animals – we think we now know why."
"It is fascinating that something with such a small mass as the alpha cells, can have such a large impact on human health" said Dr. Knudsen "We think that understanding the regulation of these cells both in healthy and diabetic individuals will improve our understanding of diabetes and provide new avenues of treatment for this growing patient population."
More information: Jakob G. Knudsen et al. Dysregulation of Glucagon Secretion by Hyperglycemia-Induced Sodium-Dependent Reduction of ATP Production, Cell Metabolism (2018). DOI: 10.1016/j.cmet.2018.10.003