Researchers standardise test for predicting transplant rejection

Researchers from The Westmead Institute for Medical Research have developed a standardised method of measuring the immune response in islet transplant recipients, helping predict patient outcomes.
Islet transplantation is a frontier therapy for type 1 diabetes with notable success in hypoglycaemic patients, where pancreatic beta cells from a donor are transplanted into a recipient, enabling the body to produce insulin, and regulate blood sugar.
Transplant recipients are given immunosuppressant medication to prevent the immune system from attacking and destroying the transplant. However, rejection may still occur in certain instances.
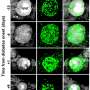
Lead researcher Dr. Min Hu and her team aimed to standardise a method using flow cytometry—technology that detects and measures the characteristics of a group of cells—to analyse the immune cells present in blood samples.
The research built on existing findings, which established that certain profiling panels (sets of characteristics that are detected and measured) could be used on flow cytometers to monitor the major immune cells involved in transplantation.
Dr. Hu said, "In the short term, islet transplant recipients do well. However, longer term, we see cases of rejection increase.
"Transplant rejection is a major cause of graft loss and loss of function. It is important that we develop a means of predicting the likelihood of rejection, so that we can intervene.
"We built on existing research and developed a consistent method of using flow cytometry to analyse the immune-cell-count, and subsets of immune cells present in the blood of transplant recipients. This involved the standardisation of a number of factors, such as sample handling and instrument set up.
"We found that this method was easy to use and produced consistent results across a number of samples.
"Importantly, we also found that this method had a very limited impact on the patient—only 1.5mL of blood was required for testing."
Islet transplantation is currently only administered in clinical trials. Dr. Hu said the research findings could be used in conjunction with current clinical trials to monitor patients after a transplant.
"Islet transplantation is an important breakthrough for people with type 1 diabetes. If the transplant is tolerated, it can significantly improve the patients' quality of life.
"Unfortunately, we currently have no method of predicting how a patient will respond to a transplant.
"By using this standardised method of flow cytometry to monitor changes in the immune system, this research could help predict whether a patient will reject a transplant, enabling early intervention, and the potential development of other solutions to stop rejection from occurring."
More information: Elvira Jimenez Vera et al, Standardisation of flow cytometry for whole blood immunophenotyping of islet transplant and transplant clinical trial recipients, PLOS ONE (2019). DOI: 10.1371/journal.pone.0217163