High BP, rising BP between ages 36-53 associated with smaller brain volume, white matter lesions in later years
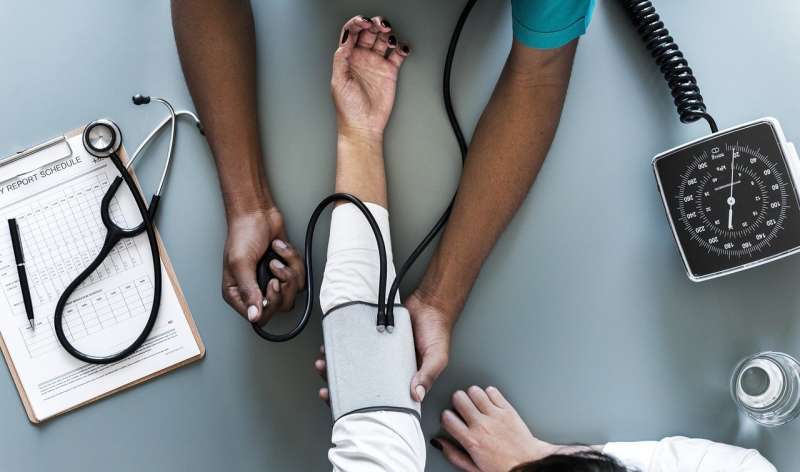
High blood pressure and large increases in blood pressure in midlife may be associated with brain pathologies in later life, according to an observational study of 502 people who have been tracked since their birth in 1946, published in The Lancet Neurology journal.
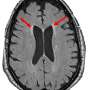
The study suggests that high blood pressure (140/90 mm Hg or higher) may lead to reductions in brain volume and higher levels of white matter hyperintensities within the brain (white matter brain lesions), but not with reduced cognition or the build-up of beta-amyloid plaques—one of the key proteins associated with Alzheimer's disease.
High blood pressure is known to increase risk for cognitive impairment later in life, but exactly how and when it increases risk is unclear. The new study tracked blood pressure from ages 36-69 to explore its influence on the brain, and found that the link may be there from a younger age than anticipated. The authors suggest that blood pressure monitoring and interventions may need to start at, or before, 40 years to maximise later brain health.
Lead author Professor Jonathan M Schott, University College London, UK, says: "Our research builds on existing evidence around the role of blood pressure and subsequent brain pathology. We found that higher and rising blood pressure between the ages of 36 and 53 had the strongest associations with smaller brain volume and increases in white matter brain lesions in later life. We speculate that these changes may, over time, result in a decline in brain function for example impairments in thinking and behaviour, so making the case for targeting blood pressure in mid-life, if not earlier."
502 participants from the Insight 46 birth cohort (born in Britain in one week in 1946) who were cognitively healthy at the age of 70 were enrolled in the study. All participants had had blood pressure taken at 36, 43, 53, 60-64, and 69 years old, and blood pressure changes between the readings were calculated.
The researchers measured each participant's overall brain volume at about 70 years of age, along with the volume of the hippocampus, the extent of white matter brain lesions, amount of beta-amyloid plaques, and cognitive capabilities.
In the cognitively normal individuals, the researchers found that having higher blood pressure at age 53 and greater increases in blood pressure between 43 and 53 were associated with having more white matter lesions at 70 (e.g. having 10mmHg higher systolic or diastolic blood pressure when aged between 43 and 53 was associated with about 7% and 15% more white matter lesions, respectively). Higher blood pressure aged 43 and greater increases in blood pressure from the age of 36 were associated with having smaller brain volumes (e.g. having a 10mmHg higher diastolic blood pressure aged 43 was associated with having a 6.9mL smaller brain at about age 70).
There was however no evidence that blood pressure affected cognition or the build-up of beta-amyloid plaques. This suggests that associations between midlife blood pressure and late-life brain health are unlikely to be occurring through the build-up of beta-amyloid, which is thought to be one of the earliest changes seen in Alzheimer's disease.
The study suggests that the fourth to sixth decades of life could be a sensitive phase when higher blood pressure and increases in blood pressure have particular impact on the future health of the brain. The authors believe that routine blood pressure measurement may need to start at, or before, 40 years old, and that different approaches to blood pressure change may be needed at different ages.
Co-author, Dr. Josephine Barnes, University College London, UK, says: "Our study design provides a unique opportunity to examine blood pressure at different ages, blood pressure changes during specific periods from early adulthood to late life, and to explore their influences on brain pathologies and brain volumes. As increases in blood pressure and higher blood pressure between the ages of 36 and 53 seem to have a detrimental effect on brain health in later life, these findings reinforce the need for monitoring blood pressure even before mid-life."
The authors highlight several limitations. As with any birth cohort, participants have gone through life phases at the same time, and will have been exposed to the same treatments and targets for blood pressure which may differ from people of different ages, meaning the results may be less generalisable to people in other age groups. The Insight 46 cohort is exclusively white British people, and additionally slightly underrepresents people with poor overall health, which reduces how these findings can be applied to different populations. The individuals included in the analyses were cognitively normal, and, as only few individuals in their early 70s have cognitive decline, the authors believe that the cognitive effects of the brain changes they observed may be seen later in life. And finally, there are other brain pathologies which can lead to dementia which further research should explore.
In a linked Comment, Dr. Lenore J Launer of the National Institute on Ageing, NIH, Bethesda, USA, states: "Although there are several major translational efforts to more completely understand the complexity of blood pressure-cognitive-related outcomes, the simple association between blood pressure and cognitive-related brain pathology is unlikely to be a chance finding. Millions of individuals have unhealthy blood pressure. Immediate attention should be given to efforts to control blood pressure through clinical services and public health interventions, and to alleviate the barriers to delivery and uptake of these messages."
More information: The Lancet Neurology www.thelancet.com/journals/lan … (19)30228-5/fulltext