Blood test identifies risk of disease linked to stroke and dementia
A UCLA-led study has found that levels of six proteins in the blood can be used to gauge a person's risk for cerebral small vessel disease, or CSVD, a brain disease that affects an estimated 11 million older adults in the U.S. CSVD can lead to dementia and stroke, but currently it can only be diagnosed with an MRI scan of the brain.
"The hope is that this will spawn a novel diagnostic test that clinicians can start to use as a quantitative measure of brain health in people who are at risk of developing cerebral small vessel disease," said Dr. Jason Hinman, a UCLA assistant professor of neurology and lead author of the paper, which is published in the journal PLoS One.
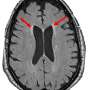
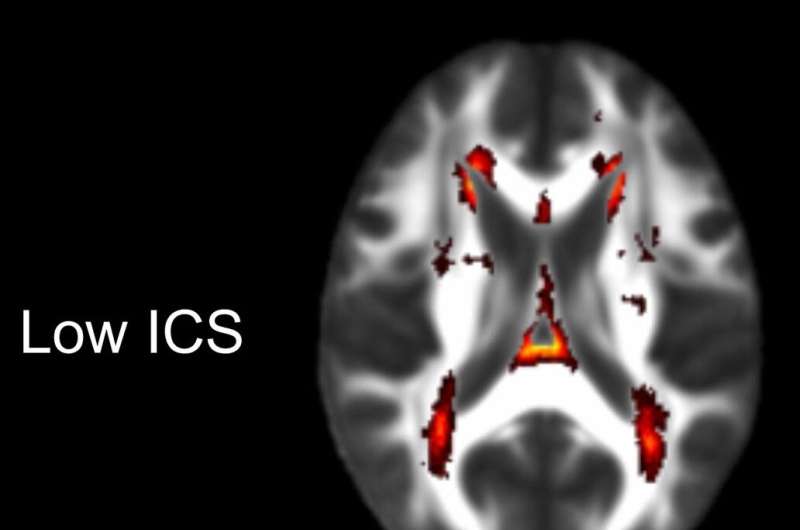
CSVD is characterized by changes to the brain's white matter—the areas of the brain that have a high concentration of myelin, a fatty tissue that insulates and protects the long extensions of brain cells. In CSVD, small blood vessels that snake through the white matter become damaged over time and the myelin begins to break down. This slows the communication between cells in the brain and can lead to problems with cognition and difficulty walking. And if the blood vessels become completely blocked, it can cause stroke.
The disease is also associated with a heightened risk for multiple forms of dementia, including Alzheimer's disease.
Typically, doctors diagnose CSVD with an MRI scan after a person has experienced dementia or suffered a stroke. About a quarter of all strokes in the U.S. are associated with CSVD. But many cases of the disease go undiagnosed because of mild symptoms, such as trouble with walking or memory, that can often be attributed to normal aging.
In the new study, Hinman and colleagues focused on six proteins related to the immune system's inflammatory response and centered on a molecule called interleukin-18, or IL-18. They hypothesized that inflammatory proteins that damage the brain in CSVD may be detectable in the bloodstream.
The researchers measured the levels of the proteins in the blood of 167 people whose average age was 76.4, and who had either normal cognition or mild cognitive impairment. As part of their voluntary participation in the study, 110 participants also underwent an MRI brain scan and 49 received a more advanced scan called diffusion tensor imaging.
People whose MRI or diffusion tensor imaging tests showed signs of CSVD had significantly higher levels of the six blood proteins, the researchers discovered. If a person had higher-than-average levels of the six inflammatory proteins, they were twice as likely to have signs of CSVD on an MRI scan and 10% more likely to very early signs of white matter damage. Moreover, for every CSVD risk factor that a person had—such as high blood pressure, diabetes, or a previous stroke—the inflammatory protein levels in their blood were twice as high, on average.
To confirm the results, the team performed the blood test in a group with a much higher risk for CSVD: 131 people who visited a UCLA Health emergency department with signs of stroke. Once again, the blood test results were correlated with white matter changes in the brain that were detected by an MRI.
"I was pleasantly surprised that we were able to associate blood stream inflammation with CSVD in two fairly different populations," Hinman said.
In MRI reports, the changes in the brain's white matter caused by CSVD are usually only categorized in general terms—as mild, moderate or severe. The blood test is a step forward, Hinman said, because it provides a more quantitative scale for evaluating the disease. That means the blood test can be used to follow the progression of the disease or to identify people who are candidates for prevention efforts or treatments for CSVD.
"We're hopeful that this will set the field on more quantitative efforts for CSVD so we can better guide therapies and new interventions," Hinman said.
The blood test is not commercially available at this time.
More information: Marie Altendahl et al. An IL-18-centered inflammatory network as a biomarker for cerebral white matter injury, PLOS ONE (2020). DOI: 10.1371/journal.pone.0227835