New insight into immune cell behavior offers opportunities for cancer treatment
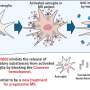
An international group of scientists has discovered that certain cells of our immune system—the so-called T cells—communicate with each other and work together as a team. To fight an infection they stimulate each other's growth, but at the same time, they inhibit each other when there is a surplus of T cells. That insight offers new opportunities for the treatment of cancer. The study is published in Immunity.
Stronger as a team
The research was led by Jan Rohr, a researcher at the Center for Chronic Immunodeficiency of the University Medical Center Freiburg. Assistant professor Joost Beltman and postdoc Margriet Palm from the Leiden Academic Centre for Drug Research collaborated on the publication. Beltman: "We looked at T cells, a particular type of immune cell. Instead of acting autonomously as individuals, these cells appear to work together as a team. And that is crucial for a healthy immune system." In order to fight an infection, it is necessary to have enough immune cells. But more does not always imply better: an excess of immune cells causes damage to healthy tissue in our body.
Communication is key
That's why T cells work together in a clever way. But successful cooperation requires communication. "We have discovered that these cells can perceive each other and communicate with each other," says Beltman. "In case of an infection, not only do other cell types give signals to T cells to multiply, but they also give them to each other." Only how do the cells know when to stop growing? "As there are more T cells, the content of the message the cells send to each other changes. As a result, a cell stops multiplying, and in that way the system regulates itself."
This insight sheds new light on immunotherapy in cancer. Tumours protect themselves by suppressing the immune system. In certain therapies, T cells are taken from a patient, strengthened and amplified in the laboratory, and finally returned to the patient. In principle, large quantities of T cells are returned for maximum effect. "It is possible that repeated doses of small quantities of T cells are more effective in combating tumour cells than a single high dose. In that case, the cells may not switch off each other, which is a risk for a high dose," explains Beltman. "But the extent to which this new insight can help improve current immune therapies needs to be further investigated."
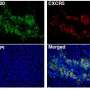
In Freiburg, the team of research leader Rohr studied immune cells in the lab using microscopic time-lapse imaging and genetic analyses. Subsequently, Beltman and Palm used the mechanisms found to create a computer model describing the interactions between cells. In this way, they demonstrated the quantitative relationship between the growth-stimulating and growth-inhibiting signals that T cells send to each other, and the number of T cells over time. "This makes it possible to predict how many T cells are active based on the signals," says Beltman. Finally, the mechanisms were tested in animal models. "These different research approaches complemented and supported each other very well," says Rohr.
More information: Simon Zenke et al. Quorum Regulation via Nested Antagonistic Feedback Circuits Mediated by the Receptors CD28 and CTLA-4 Confers Robustness to T Cell Population Dynamics, Immunity (2020). DOI: 10.1016/j.immuni.2020.01.018