How a specific population of lymphocytes promotes autoimmune disease
Researchers from Karolinska Institutet in collaboration with a lab in San Antonio U.S., have uncovered how a specific population of lymphocytes promotes autoimmune disease by giving up their regulatory role in the immune system. The newly discovered mechanism is published in PNAS from research led by Dr. Saikiran Sedimbi and Prof. Mikael Karlsson.
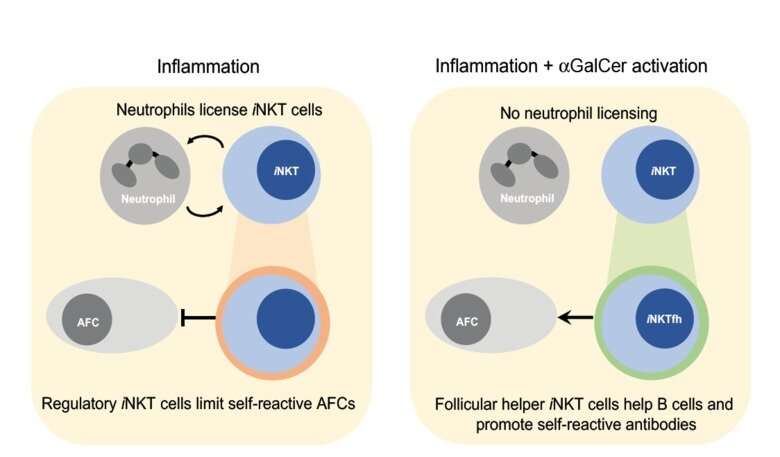
Autoimmune disease is a result of an imbalance of the immune system that includes breakdown of several mechanisms that normally prevent disease. The groups working at Biomedicum now discovered that a population of cells that normally block autoimmunity can switch function to instead promote disease. This is due to a combination of inflammation and specific stimulation through glycolipids. The study shows that a group of lymphocytes known as iNKT cells, that normally prevent autoreactive B cells from secreting pathogenic antibodies, lost this ability and instead took on the role of supporting these B cells. This included loss of interaction with neutrophils that normally regulate their function and enhancement of Rheumatoid Arthritis (RA) in a model of this disease.
The team identified a switch in iNKT cells when they were stimulated with glycolipid agonist alpha-galactosylceramide (aGalCer) and the inflammatory cytokine IL-18. iNKT cells displayed lower levels of the transcription factor GATA3 and simultaneously an increase in the transcription factor BCL6, together with cell surface expression of CXCR5 and PD-1, a classical follicular T helper phenotype. This phenotype promoted germinal center B cell responses that resulted in immunoglobulin (Ig) class switch. The authors also observed an increase in autoreactive anti-DNA antibodies belonging to the subclasses IgG2b, IgG3 and IgE. Using a reporter system where B cells that undergo the germinal center response upregulate human specific markers, the authors demonstrate that combined glycolipid and inflammatory stimulation of iNKT cells in vivo, results in more B cell undergoing the GC response. Also, normally regulatory iNKT cells interact with neutrophils to regulate B cells but the authors found that this interaction was lost during this switch in function (Figure 1). To validate that this switch in iNKT cells was sufficient to drive autoimmunity, the team used a model for collagen-induced arthritis, where co-administration of aGalCer and IL-18 resulted in early onset RA and increased immune cell activation.
These results show how autoimmune disease can occur and how safety mechanisms in the immune system can be disrupted. In addition, it provides knowledge that can be used to restore balance and treat autoimmunity.
More information: Saikiran K. Sedimbi et al. Combined proinflammatory cytokine and cognate activation of invariant natural killer T cells enhances anti-DNA antibody responses, Proceedings of the National Academy of Sciences (2020). DOI: 10.1073/pnas.1920463117