Rifampin regimen found to be cheaper than isoniazid for latent tuberculosis
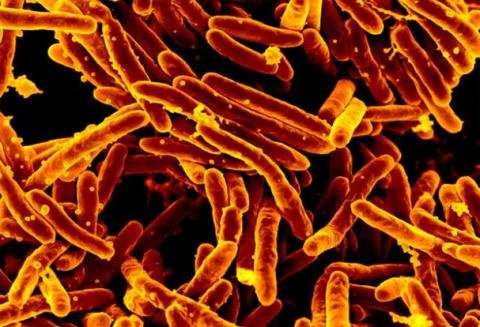
A 4-month rifampin regimen was found to be cheaper than a 9-month course of isoniazid for the treatment of latent tuberculosis in a cost-comparison study published in the Annals of Internal Medicine. Currently, isoniazid is the standard of treatment in most countries for latent tuberculosis infection. The finding that 4 months rifampin treatment is cheaper adds to previously published evidence that this treatment is as effective, while also significantly safer and more likely to be completed, than 6 months or 9 months isoniazid treatment. These findings have the potential to change the way latent tuberculosis is treated.
An estimated one quarter of the global population has latent tuberculosis infection. If left untreated, 10 percent of these 1.7 billion people will develop tuberculosis disease. Latent tuberculosis infection treatment is not new. Monotherapy with isoniazid for 6 to 12 months has been long proven to reduce the risk for developing active tuberculosis by up to 90 percent. The long treatment duration and the fear of serious, even fatal adverse events have limited acceptance and completion.
Researchers from McGill University studied data from two multicenter randomized clinical trials conducted in adults and children with risk factors for developing tuberculosis. They compared health care use and associated costs of treatment with 4 months of rifampin and 9 months of isoniazid in these studies. The analysis indicated that latent tuberculosis infection treatment with 4 months of rifampin resulted in less health service use and significantly lower costs than 9 months of isoniazid for both adults and children. These trials included participants from diverse treatment settings in 9 countries. According to the researchers, these findings suggest that tuberculosis programs in all countries should consider adoption of the 4-month rifampin regimen as a first-line therapy for latent tuberculosis infection.
More information: Annals of Internal Medicine (2020). https://www.acpjournals.org/doi/10.7326/M19-3741