Balance dysfunction after traumatic brain injury linked to diminished sensory acuity

Kessler Foundation researchers have linked balance dysfunction in individuals with traumatic brain injury with diminished sensory acuity. This study used a psychophysical approach to develop a new metric called the perturbation perception threshold (PPT) for objectively quantifying impaired sensory acuity after traumatic brain injury. The article, "Evaluating sensory acuity as a marker of balance dysfunction after a traumatic brain injury: A psychophysical approach" (doi: 10.3389/fnins.2020.00836), was published August 11, 2020 in Frontiers in Neuroscience.
The authors are Rakesh Pilkar, Ph.D., Kiran Karunakaran, Ph.D., Akhila Veerubhotla, Ph.D., Naphtaly Ehrenberg, MS, Oluwaseun Ibironke, and Karen Nolan, Ph.D., from the Center for Mobility and Rehabilitation Engineering Research at Kessler Foundation.
Balance problems limit independence, and increase the risk of falls and/or injury after traumatic brain injury. To improve rehabilitation interventions, more knowledge is needed about the integration of the visual, vestibular and somatosensory factors that contribute to balance, and how brain injury can adversely affect this complex system of balance control.
Despite the importance of accurately perceiving external perturbations to maintaining balance, limited research has been done on the contributions of sensory acuity to balance dysfunction after traumatic brain injury, according to lead author Dr. Pilkar, the research scientist who directs the Center's Balance Assessment and Training Laboratory.
Study investigators sought to quantify the threshold for perceiving perturbation in individuals with and without traumatic brain injury, and determine the influence on static and dynamic balance. They provoked body sway during standing and measured response thresholds. Lower thresholds for perceiving these perturbations indicate better body awareness to maintain balance in dynamic settings.
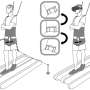
Participants included ten individuals with traumatic brain injury (TBI group) and 11 healthy controls (control group), all of whom underwent comprehensive baseline balance assessment (Berg Balance Scale, Timed-Up and Go, 5-min Walk Test, and 10-meter Walk Test). Using a responsive platform called the Neurocom Smart Equitest Clinical Research System, researchers delivered measured stimuli in three frequencies that briefly moved the platform in an anterior-posterior direction. Participants were asked to respond to 21 trials randomized for movement (perturbation) or no movement (nonperturbation). Each individual's responses to these trials were recorded while standing on the platform, to establish their PPT.
Results revealed significant differences in PPT between the TBI and control groups. Compared with the control group, the TBI group had higher PPT and lower functional scores on static and dynamic balance. While further research is needed, these findings have important implications for the rehabilitation of individuals with TBI. "As a means of detecting and quantifying sensory acuity PPT may serve as a novel marker for the sensory integration deficits that underlie balance impairments in individuals recovering from traumatic brain injury," said Dr. Pilkar. "This line of research will provide the information we need to develop new rehabilitative treatments that restore balance and reduce the risk for falls, and improve long-term outcomes after traumatic brain injury."
More information: Rakesh Pilkar et al, Evaluating Sensory Acuity as a Marker of Balance Dysfunction After a Traumatic Brain Injury: A Psychophysical Approach, Frontiers in Neuroscience (2020). DOI: 10.3389/fnins.2020.00836