Study may explain the microbiome-immunotherapy connection
Cancer immunotherapy may get a boost from an unexpected direction: bacteria residing within tumor cells. In a new study published in Nature, researchers at the Weizmann Institute of Science and their collaborators have discovered that the immune system "sees" these bacteria and shown they can be harnessed to provoke an immune reaction against the tumor. The study may also help clarify the connection between immunotherapy and the gut microbiome, explaining the findings of previous research that the microbiome affects the success of immunotherapy.
Immunotherapy treatments of the past decade or so have dramatically improved recovery rates from certain cancers, particularly malignant melanoma; but in melanoma, they still work in only about 40% of the cases. Prof. Yardena Samuels of Weizmann's Molecular Cell Biology Department studies molecular "signposts"—protein fragments, or peptides, on the cell surface—that mark cancer cells as foreign and may therefore serve as potential added targets for immunotherapy. In the new study, she and colleagues extended their search for new cancer signposts to those bacteria known to colonize tumors.
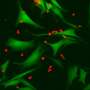
Using methods developed by departmental colleague Dr. Ravid Straussman, who was one of the first to reveal the nature of the bacterial "guests" in cancer cells, Samuels and her team, led by Dr. Shelly Kalaora and Adi Nagler (joint co-first authors), analyzed tissue samples from 17 metastatic melanoma tumors derived from nine patients. They obtained bacterial genomic profiles of these tumors and then applied an approach known as HLA-peptidomics to identify tumor peptides that can be recognized by the immune system.
The research was conducted in collaboration with Dr. Jennifer A. Wargo of the University of Texas MD Anderson Cancer Center, Houston, Texas; Prof Scott N. Peterson of Sanford Burnham Prebys Medical Discovery Institute, La Jolla, California; Prof Eytan Ruppin of the National Cancer Institute, U.S.; Prof Arie Admon of the Technion—Israel Institute of Technology and other scientists.
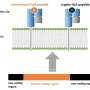
The HLA peptidomics analysis revealed nearly 300 peptides from 41 different bacteria on the surface of the melanoma cells. The crucial new finding was that the peptides were displayed on the cancer cell surfaces by HLA protein complexes—complexes that are present on the membranes of all cells in our body and play a role in regulating the immune response. One of the HLA's jobs is to sound an alarm about anything that's foreign by "presenting" foreign peptides to the immune system so that immune T cells can "see" them. "Using HLA peptidomics, we were able to reveal the HLA-presented peptides of the tumor in an unbiased manner," Kalaora says. "This method has already enabled us in the past to identify tumor antigens that have shown promising results in clinical trials."
More information: Shelly Kalaora et al. Identification of bacteria-derived HLA-bound peptides in melanoma, Nature (2021). DOI: 10.1038/s41586-021-03368-8