New study gives clue to the cause, and possible treatment of Parkinson's disease
Researchers from the Brain Research Institute, Niigata University, Japan may have unraveled a new approach that could revolutionize the treatment, prevention, and possibly reversal of the damage that could lead to Parkinson's disease (PD). This novel finding utilizing cellular and zebrafish models, demonstrates how the leakage of mitochondrial dsDNA into the cytosol environment of the cell can contribute to the impairment of brain tissue of patients with PD.
Parkinson's disease is the second most common neurodegenerative disease, and its prevalence has been projected to double over the next 30 years.
These sobering statistics and the quest for PD prognostic marker discovery inspired a team of scientists led by Prof. Hideaki Matsui to build upon previous knowledge that link mitochondrial dysfunction and lysosomal dysfunction to PD. In an interview Prof. Matsui said, "Our results showed for the first time that cytosolic dsDNA of mitochondrial origin leaking and escaping from lysosomal degradation can induce cytotoxicity both in cultured cells, as well as in zebrafish models of Parkinson's disease."
Prof. Matsui went on to explain that "This study showed that the leakage of this mitochondrial nucleic material may occur as a result of mitochondrial dysfunction, which may involve genetic mutations in genes encoding mitochondrial proteins or incomplete degradation of mitochondrial dsDNA in the lysosome—which is a 'degradation factory' of the cell. Upon the leakage into the cytoplasm, this undegraded dsDNA is detected by a foreign DNA sensor of the cytoplasm (IFI16) which then triggers the upregulation of mRNAs encoding for inflammatory proteins (type I interferon stimulated cytokines such as IL1β). Although further investigation is required, we hypothesize that the subsequent accumulation of inflammatory protein within the cytoplasm, may cause cell functional imbalance and ultimately cell death."
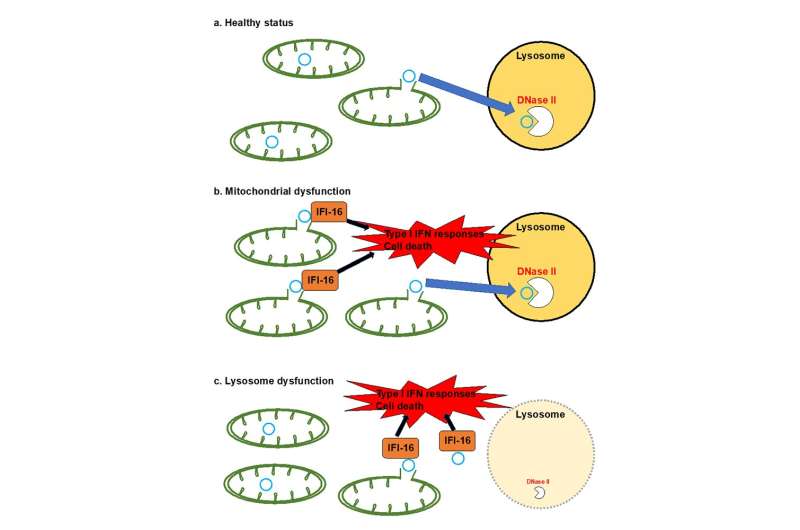
"However, this dsDNA leakage effect can be counteracted by DNAse II, a dsDNA degrading agent.", Prof. Akiyoshi Kakita, who was an associate investigator in the study also added.
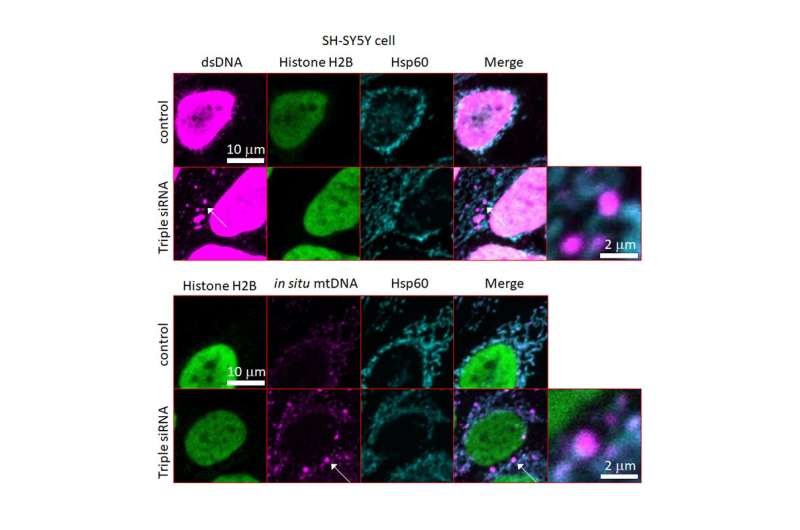
The first part of the study was conducted in vitro, using cells of nerve cancer origin (SH-SY5Y cells) with defective mitochondria and lysosomal dysfunctions through knockdown of GBA, ATP13A and PINK1 genes. The mutant cells demonstrated leakage of dsDNA and accumulation of inflammatory cytokines and cell death. In an additional comparison experiment using mutant cells (with defective mitochondrial proteins) and wild type SH-SY5Y cells, they further demonstrated that DNAse II rescued cells through the degradation of dsDNA.
In a confirmatory study using a PD zebrafish model (gba mutant), the researchers demonstrated that a combination of PD-like phenotypes including accumulation of cytosol dsDNA deposits, reduced number of dopaminergic neurons after 3 months. Lastly, they further generated a DNase II mutant zebrafish model which exhibited decreased numbers of dopaminergic neurons and demonstrated accumulated cytosolic DNA. Interestingly, when then gba mutant zebrafish was complemented with human DNAse II gene, the overexpression of human DNAse II decreased cytosolic dsDNA deposits, rescued neuro-degradation by rescuing the number of dopaminergic and noradrenergic neurons after 3 months.
This demonstrated that neurodegenerative phenotype of gba mutant zebrafish induced by dsDNA deposits in the cytosol can be restored by DNAse II.
In a step further, to determine the effect of cytosolic dsDNA of mitochondrial origin in human brain with PD, they inspected postmortem human brain tissues from patients who were diagnosed with idiopathic PD. They observed abundance of cytosolic dsDNA of mitochondrial origin in medulla oblongata of postmortem brain tissues, the levels of IFI16 were also markedly increased in these brain tissues. Taken together, results in this study demonstrated that cytosolic dsDNA of mitochondrial origin accumulated in PD brains and that these dsDNA deposits and IFI16 play contributory roles in human PD pathogenesis.
More information: Hideaki Matsui et al, Cytosolic dsDNA of mitochondrial origin induces cytotoxicity and neurodegeneration in cellular and zebrafish models of Parkinson's disease, Nature Communications (2021). DOI: 10.1038/s41467-021-23452-x


















