Experimental and computational synergy—Promising COVID-19 results
An international collaboration between researchers from the Center for Cooperative Research in Biosciences (CIC bioGUNE, Bilbao), the Luxembourg Centre for Systems Biomedicine (LCSB) at the University of Luxembourgand and the Department of Immunology of St Jude Children's Research Hospital (Kanneganti Lab, Memphis) highlights how fostering synergies between computational and experimental studies can lead to important results in the field of immunology. In an article published in November in Trends in Immunology, researchers illustrate the potential of this type of collaboration through recent results obtained on the modulation of hyperinflammation in COVID-19. Both a computational approach led by Prof. Antonio Del Sol and an experimental study led by Dr. Thirumala-Devi Kanneganti showed that a specific protein could help modulate COVID-19-induced lung hyperinflammation. Building on this success, the authors detail how experimental and computational approaches can support each other and advocate for coordinated efforts to accelerate the discovery of new therapeutic targets.
A promising new approach
Thanks to the large amount of -omics data becoming increasingly available, sophisticated computational models are developed for new fields such as immunology and the predictions they generate will help identify key molecules in inflammatory processes. The application of such computational systems biology approaches to immunology could lead to novel and more efficacious therapeutic strategies. "The recent work of our two teams on the modulation of hyperinflammation in COVID-19 illustrates really well how the synergy between experimental and computational researchers can accelerate the discovery of molecules of interest," explains Prof. Antonio Del Sol, head of the Computational Biology groups at the LCSB and CIC bioGUNE. "By using computational modeling to inform traditional experimental approaches, we confirmed in a few months a potential target for medical intervention in COVID-19 patients. This is indeed very promising."
Understanding the "cytokine storm" in COVID-19
In recent studies, researchers from the LCSB and CIC bioGUNE—on the computational side—and from the Kanneganti Lab at St. Jude Children's Research Hospital—on the experimental side—focused on the mechanisms underlying the hyperinflammatory response in COVID-19. Hyperinflammation is caused when the immune response is amplified and maintained by positive feedback loops above the level needed to control disease. Kanneganti's lab recently found that in COVID-19, as well as other diseases, this hyperinflammatory "cytokine storm" could be mechanistically defined as a life-threatening condition caused by excessive production of proinflammatory proteins, cytokines, mediated by a form of inflammatory cell death called PANoptosis. In COVID-19, PANoptosis and the concomitant cytokine storm cause organ damage and increase the severity of the symptoms. This makes treatment challenging, as therapeutics need to alleviate inflammation while maintaining the patient's ability to clear the virus through cell death and other pathways. It is therefore crucial to identify the molecules that amplify and maintain the inflammatory response. It is the first step towards new and putative life-saving therapeutic strategies.
Two studies identify protein TLR2 as a target
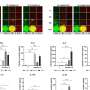
In a first study published in Science Advances, researchers from the Computational Biology groups of the LCSB and CIC bioGUNE used a novel computational method to analyse over 1700 cell-cell interactions and create a comprehensive map of the immune response in the lungs of COVID-19 patients. Their model identified Toll-like Receptor 2 (TLR2) as a molecule that might be able to modulate the inflammatory response, predicting that the inhibition of this protein could disrupt up to 75% of the feedback loops without interfering with the general immune response. The study put TLR2 on the map as a potential target for medical intervention in severe COVID-19 cases.
Separately, the team of Dr. Thirumala-Devi Kanneganti from the Department of Immunology of St Jude Children's Research Hospital published a study in Nature Immunology that independently suggested that TLR2 might act as a key modulator of COVID-19-induced hyperinflammation. Using in vitro and in vivo experiments, the researchers found that increased expression of TLR2 in the blood of patients with COVID-19 correlated with disease severity and that, upon infection by the virus, TLR2 mediated the production of cytokines. The study also showed that treatment of transgenic mice with a TLR2 inhibitor protected the animals against SARS-CoV-2-mediated inflammatory cytokine production and mortality. "Experimental validation of computationally derived biomarkers is critical to provide multiple lines of evidence to support the proof-of-concept for the utility of targeting TLR2 to modulate inflammation. It is imperative to combine computational and experimental approaches to understand mechanisms involved in inflammatory processes," underlines Dr. Kanneganti.
A coordinated effort to achieve full potential
This example is far from the only one: In a growing number of studies, systems immunology approaches are being successfully employed to help predict novel therapeutic targets for modulating uncontrolled immune responses. "Computational modeling and experimental validation will become key partnerships in biomedical research and should be systematically developed to achieve their full potential," details Dr. Ilya Potapov, member of the Computational Biology group at the LCSB.
In their recent paper published in November in Trends in Immunology, the three co-authors mention the challenges researchers will have to tackle when building computational models in the context of hyperinflammation—such as technological limitations, shortage of good experimental models and mutual unawareness—and postulate that experimental and computational efforts should be synergised from the onset. "The technological advances have set the stage for us. Now, we need to work together to build accurate computational models, define the necessary data and design experiments to validate the computational predictions. This is the key to designing novel and more efficacious therapeutic strategies," concludes Prof. Del Sol.
More information: Ilya Potapov et al, Fostering experimental and computational synergy to modulate hyperinflammation, Trends in Immunology (2021). DOI: 10.1016/j.it.2021.11.004