Improving diet management for cancer patients
A new dietary tool to quickly and accurately assess micronutrient levels aims to help cancer patients fight disease, paving the way to find better nutritional solutions for oncology services, Flinders University researchers say.
Chronic inflammation is a risk factor for cancer, the leading cause of death globally with 10 million cancer deaths and 19.3 million new cases in 2019.
"Dietary intake, specifically consumption of anti-inflammatory micronutrients, can play a role in both cancer initiation as well as the treatment-related outcomes experienced by patients receiving systemic cancer therapy," says Flinders University Ph.D. candidate Mitali Mukherjee, an accredited practicing dietitian at Flinders Medical Centre.
"Diet and nutritional choices are important in oncology and should be carefully managed. Some cancer patients don't get their diet history checked unless they are losing weight or are referred to a dietitian but dietary micronutrient intakes are rarely assessed in a clinical setting," she says.
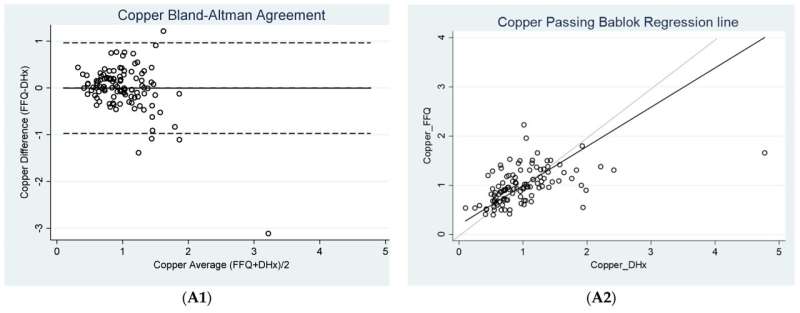
"Tested by 112 cancer patients, our 21-item food frequency questionnaire for 14 common micronutrients can be done in about 10 minutes and could be used to screen patients having suboptimal micronutrient intakes.
"We hope it will pave a pathway for provision of dietary advice in clinical practice and future observational research with chemotherapy and immunotherapy cancer treatments."
Ms Mukherjee, with other SA Health and Flinders University experts including Professor Michelle Miller and medical oncologist Dr. Shawgi Sukumaran, hopes to expand the study to use the tool to test the validity of anti-inflammatory nutrients among oncology patients receiving systemic treatment.
The tool tested adequacy of a patient's micronutrients for 12 nutrients include copper, iron, vitamins A, E, and D, alpha linolenic acid, long-chain omega 3 fatty acids (LC n3-FA), arginine, glutamic acid, isoleucine, leucine, and valine.
"Further research could help to determine whether micronutrient intakes and an anti-inflammatory diet can aid in altering the tumor microenvironment, reduce inflammatory side effects and immune-related adverse events," says senior author Dr. Sukumaran.
Dietary factors have been associated with risk of developing cancers, especially breast, colorectal, head or neck, lung and prostate. Dietary factors also play a role in side effects and chemotherapy and other treatment options for cancers.
Previous studies have confirmed the benefits of a lower dietary inflammatory index score associated with a Mediterranean or less processed or refined foods comprising large amounts of fruits and vegetables, lean meats, fish, wholegrains and healthy fats.
Ms Mukherjee says there is currently no validated tool to measure micronutrient intakes in a clinical setting. "Collecting comprehensive dietary information from a diet history and analyzing it with Foodworks software can take up to two hours to assess micronutrient intakes, which is generally not feasible in clinical practice," she says.
The article, "Validation of a Short Food Frequency Questionnaire to Measure Dietary Intake of a Selection of Micronutrients in Oncology Patients Undergoing Systemic Therapy," has been published in Nutrients.
More information: Mitali S. Mukherjee et al, Validation of a Short Food Frequency Questionnaire to Measure Dietary Intake of a Selection of Micronutrients in Oncology Patients Undergoing Systemic Therapy, Nutrients (2021). DOI: 10.3390/nu13124557
















