This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Explaining why some patients may test positive for COVID-19 long after recovery
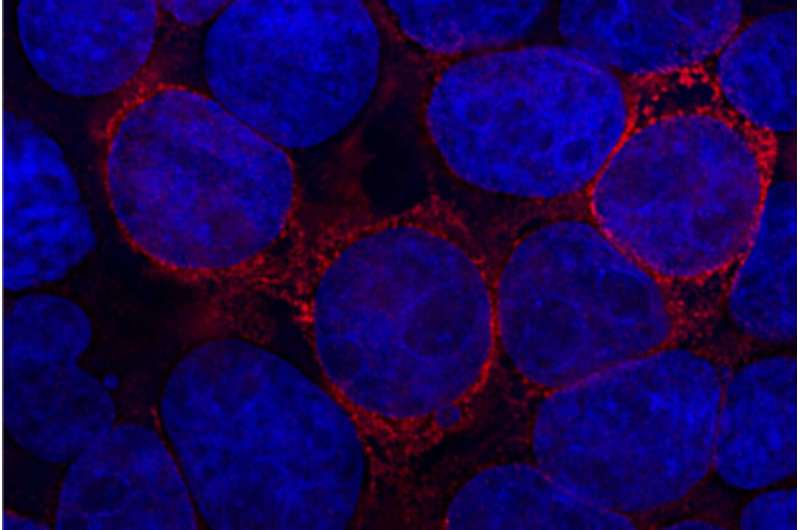
SARS-CoV-2, the virus that causes COVID-19, seems to have become a permanent presence in our lives. Research from Whitehead Institute Founding Member Rudolf Jaenisch's lab reveals that this may be true on multiple levels. Jaenisch, postdoc Liguo Zhang, and colleagues have shown that when the virus infects people, it is capable of integrating parts of its genetic code into the human genome through a process called reverse transcription. This genomic integration is rare, but due to how many hundreds of millions of people have been infected, it has likely occurred many times.
In a paper published in the journal Viruses on February 25, the researchers use and compare multiple methods to show that SARS-CoV-2 can integrate into host cells' genomes. The paper is a follow up to Jaenisch and Zhang's 2021 paper in the Proceedings of the National Academy of Sciences, which provided initial evidence of SARS-CoV-2 genomic integration.
The original paper intended to solve the puzzle of why some people who had had COVID-19 were still testing positive long after recovering from the disease. The answer the researchers found was that parts of the viral genome were reverse transcribed into the human genome, meaning the viral RNA was transcribed or "read" into DNA (a reverse of the usual process) and then that DNA was stitched into the cell's DNA. Then, when the cells' genomes were transcribed into RNA, the portion of the virus' genome that had been incorporated would be included and could be recognized by a PCR test, leading to a positive result.
In order to further substantiate the findings described in the previous paper, Jaenisch and Zhang have now performed additional experiments and analyses. The new paper explains why some experiments testing for viral genomic integration would come up with a negative result, and how this is consistent with Jaenisch and Zhang's conclusion. Additionally, Jaenisch and Zhang examine whether viral RNA put into cells, as a model of the COVID-19 mRNA vaccines, can also integrate into the human genome, and find initial evidence that it cannot.
"This paper puts our data on a very firm footing," Jaenisch says. "Hopefully, it will clarify some of the issues raised in the discussion that followed the first paper, and provide some reassurance to people who were worried about the implications for the vaccine."
Hunting for a needle in a haystack
The main challenge in finding evidence of SARS-CoV-2 integrating into the human genome is that this event appears to be very rare. In the new paper, Jaenisch and Zhang used digital PCR, an approach that can sensitively detect specific DNA sequences in cells, to see how commonly the sequence that they would find in instances of viral RNA being read into DNA appeared in infected cells. Specifically, they looked for reverse transcribed SARS-CoV-2 complementary DNA (cDNA), DNA that is made from the virus' original mRNA.
Digital PCR revealed that for every one thousand cells, reverse transcribed viral cDNA was only present in around four to twenty cells. This number includes all detected instances of viral cDNA, whether integrated into the genome or not, so genomic integration is likely even rarer—indeed, the new research suggests that only a fraction of the total cDNA identified is from genomic integration.
Because genomic viral integration is so rare, Jaenisch and Zhang needed to use multiple complementary methods to test for it. One approach, called whole genome sequencing (WGS), is able to search cells' genomes in great detail. When it does come across an instance of viral genomic integration, it can identify not only the reverse transcribed viral sequence, but also two sequences near the viral sequence that are added when it is integrated into the genome by a common reverse transcription complex called LINE1, which is encoded in the host cells.
The combination of viral cDNA plus the two nearby cellular host sequences provides very strong evidence that viral cDNA is not only present but has been incorporated into the cell's genome. However, WGS can only search the equivalent of a few cells' genomes, and so when searching for a rare event, like SARS-CoV-2 integration, it often comes up empty. People skeptical of the first paper performed this type of experiment and came up with a negative result; Jaenisch and Zhang were not surprised by that, and it is consistent with their own findings when using this approach.
"Because the human cell genome coverage by whole genome sequencing is very limited, you would need to run the sequencing experiment many times in order to have a good chance of detecting one viral genome copy," Zhang says.
In order to make the most of WGS, Jaenisch and Zhang induced their cells to overexpress LINE1, the cellular machinery that reverse transcribes viral RNA into the human genome. This exponentially increases the amount of viral cDNA that gets made; when the researchers performed digital PCR on their cells with overexpression, it detected fourteen to twenty thousand cDNA copies per thousand cells. Consequently, WGS was able to detect instances of viral cDNA plus the two nearby sequences that are the telltale signature of genomic integration in these cells.
"This is unambiguous proof of viral genomic integration," Zhang says.
This type of experiment is called a positive control. Researchers use it to prove that, in ideal circumstances, the biological phenomenon they are curious about can occur. The question then becomes: does the phenomenon happen in normal circumstances? This was a criticism raised by some researchers in response to the first paper: they were not convinced that viral genomic integration happens in the cells of an infected person, which do not have the same levels of LINE1.
The search gets shallower but wider
Jaenisch and Zhang used another approach to hunt for evidence of viral genomic integration in cells without LINE1 overexpression. The approach, called an enrichment method and performed with the tool TagMap, can analyze thousands of cells—enough cells to reliably find evidence of a rare event. However, it cannot get the same detail as whole genome sequencing; TagMap enriches and captures shorter sequences of DNA, so it can only capture one of the two nearby sequences that act as a signature alongside viral cDNA. However, the smaller stretch of DNA that the researchers focused on still has features that can be used as evidence of integration. With this approach, Jaenisch and Zhang detected many instances of viral cDNA linked to the nearby cellular sequence.
Jaenisch and Zhang argue that the combined results of these experiments show strong proof of viral integration. Whole genome sequencing provides very strong proof that viral genomic integration can occur in the right conditions. Enrichment with TagMap provides reasonably strong proof that viral genomic integration occurs in normal cells.
"Each of these methods has advantages and disadvantages. You have to combine them to get the complete picture," Jaenisch says.
Turning to the vaccine
After reaffirming their results that genomic integration of SARS-CoV-2 happens following viral infection, the researchers wanted to know whether the same thing happens with mRNA from the COVID-19 vaccines—which had been a concern expressed by many in the wake of the first paper. Jaenisch and Zhang could not get access to the actual vaccine RNA, packaged into a lipid coat, which is used for vaccination. Instead, they created a model of vaccine injection, inserting a bit of SARS-CoV-2 genetic material (mRNA) into cells through transfection, or non-infection "delivery" of genetic content into cells.
The researchers found that transfection of SARS-CoV-2 mRNA did not lead to genomic integration in the same way that infection did. Infection naturally produces a large amount of viral RNA and causes an inflammatory response in cells. Such cellular stresses increase the level of the reverse transcription machinery. Transfection does not do this, and correspondingly, the researchers found no evidence with TagMap that it led to viral genomic integration by LINE1 in normal cells.
The researchers' model of vaccine injection is missing several key features of the actual vaccine. In the future, Jaenisch hopes to follow up on this research using the actual vaccine RNA sequence, and testing in an animal model to more closely match what happens during vaccine injection. In the meantime, the researchers hope that these initial results are reassuring.
"We need to do further testing, but our results are consistent with vaccine RNA not integrating," Jaenisch says.
More information: Liguo Zhang et al, LINE1-Mediated Reverse Transcription and Genomic Integration of SARS-CoV-2 mRNA Detected in Virus-Infected but Not in Viral mRNA-Transfected Cells, Viruses (2023). DOI: 10.3390/v15030629