This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Research identifies mechanisms for selective multiple sclerosis treatment strategy
The Wistar Institute's Paul M. Lieberman, Ph.D., and lab team led by senior staff scientist and first author Samantha Soldan, Ph.D., have demonstrated how B cells infected with the Epstein-Barr virus (EBV) can contribute to a pathogenic, inflammatory phenotype that contributes to multiple sclerosis (MS). The group has also shown how these problematic B cells can be selectively targeted in a way that reduces the damaging autoimmune response of multiple sclerosis.
The lab's findings are published in Nature Microbiology in a paper titled "Multiple sclerosis patient derived spontaneous B cells have distinct EBV and host gene expression profiles in active disease."
EBV—a usually inactive (latent) herpesvirus—affects most of the human population; more than 90% of people carry the virus as a passive, typically symptomless infection. However, EBV infection has been linked to several diseases, including MS, an incurable, chronic autoimmune disease that causes the body's immune system to attack the myelin sheath of neurons in the brain and nervous system.
Because myelin sheathing facilitates fast nervous system signaling (the fatty insulation of myelin along a neuron's axon allows electrical impulses to travel through neuronal networks faster), its degradation can cause a wide variety of symptoms in both type and severity that may include motor control disruption, sensory issues, and speech difficulties.
Though researchers know that EBV can contribute to the development of MS, the exact mechanisms by which it does so aren't completely understood. The Lieberman lab, in seeking to understand how EBV contributes to the development of MS, collaborated with Steven Jacobson, Ph.D., of the Neuroimmunology Branch at the National Institute of Neurological Disorders and Stroke, who contributed cell line samples from patients.
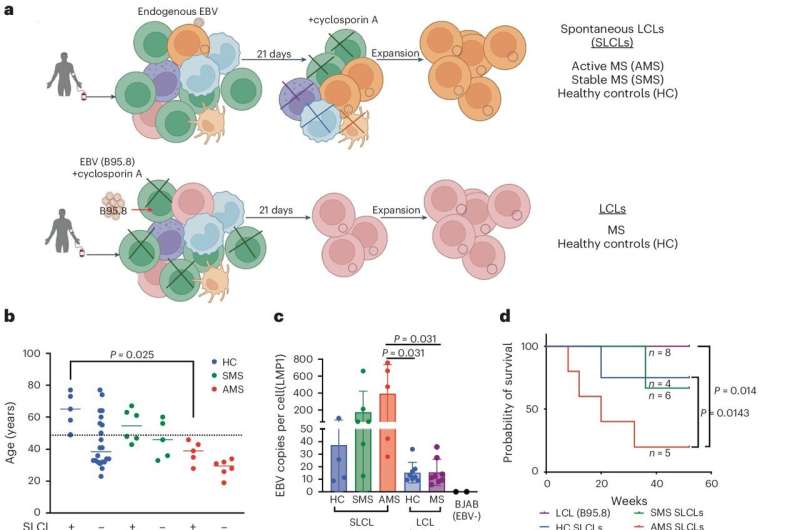
The research team analyzed spontaneous lymphoblastoid cell line (SLCL) cell samples from a healthy control group; a group of patients with active MS (as opposed to so-called stable MS; the disease is characterized by unpredictable periods of flare-ups and eased symptoms); and a group of patients with stable MS.
B cells are crucial cells of the immune system that help regulate the body's immune responses; they have also been implicated in autoimmune conditions due to their role as mediators of which biological signals warrant immune response.
And B cells, when infected with EBV, become immortalized—that is, the cells are no longer constrained by senescence, so they can continue to divide an indefinite number of times—as "lymphoblastoid cell lines," or LCLs. This immortalized B cell state can occur spontaneously within the body as a result of EBV infection, which is how the Lieberman lab was able to extract immortalized SLCL samples for study from the different patient groups.
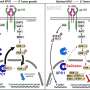
Having obtained the matched samples, Dr. Lieberman and his team conducted genetic analyses of the SLCLs and confirmed that the MS-positive sample groups showed greater expression of genes associated with lytic EBV ("lytic" describes when latent viruses like EBV become active); they also saw increased inflammatory signaling and expression of the FOXP1 protein, the latter of which was shown to promote lytic EBV gene expression. As a whole, the group's findings suggested a mechanism of lytic EBV in MS that promoted inflammation and disease.
Diving further, Lieberman's group tested several antiviral compounds on all SLCL groups and found that one, TAF, reduced lytic EBV gene expression without killing the cells. TAF also significantly reduced the expression of inflammatory cytokines like IL-6 in the SLCLs from the patients with active MS.
Finally, when cultured SLCLs from active MS, stable MS, and controls were administered TAF in the presence of antiviral T cells, the T cell response (a major factor in the autoimmune dysfunction of MS) was reduced in SLCLs from patients with MS but not reduced in the control SLCLs—an indication that TAF treatment has potential as a selectively cytotoxic anti-lytic treatment for MS.
"Our work with these SLCLs shows that the problematic inflammation signaling from lytic EBV can be selectively targeted in a way that demonstrably reduces damaging immune responses," said Dr. Lieberman. "We're excited about expanding this concept further; we have the potential to see whether TAF or other inhibitors of EBV might be a viable treatment for multiple sclerosis that can stop the autoimmune damage without causing wide-ranging and dangerous cell death."
More information: Samantha S. Soldan et al, Multiple sclerosis patient-derived spontaneous B cells have distinct EBV and host gene expression profiles in active disease, Nature Microbiology (2024). DOI: 10.1038/s41564-024-01699-6