Could a cancer drug potentially prevent learning disabilities in some kids?
A drug originally developed to stop cancerous tumors may hold the potential to prevent abnormal brain cell growth and learning disabilities in some children, if they can be diagnosed early enough, a new animal study suggests.
The surprising finding sets the stage for more research on how anti-tumor medication might be used to protect the developing brains of young children with the genetic disease neurofibromatosis 1—and other diseases affecting the same cellular signaling pathway.
The findings, made in mice, are reported in the journal Cell by scientists at the University of Michigan Medical School and their colleagues. The results are also important to understanding the stem cells that become different brain cells.
Neurofibromatosis 1, or NF1, affects one in every 3,000 children, and causes benign tumors to grow throughout the body, large head size and other issues. Many children with NF1 also struggle with learning to read, write, do math and behave well.
This impact on brain function is considered the most common serious issue caused by NF1, and often appears before other symptoms, except for brown patches on the skin that are often mistaken for birthmarks. But while the tumors that erupt mostly later in life have been well-studied, NF1's effect on brain function isn't understood.
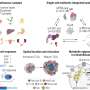
In the new paper, the team studied neural stem cells – a kind of master cell that can become any type of neural tissue. In newborn mice with two copies of the genetic mutation that causes NF1, neural stem cells in a key area of the brain were far more likely to produce a kind of "helper" nerve cell called glia. They produced far fewer cells called neurons, which send and receive crucial signals in the brain and body.
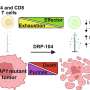
The scientists then took aim at this abnormal cell growth by giving the mice an experimental drug that has already been used in clinical trials for advanced cancer. Called PD0325901, the drug blocks a specific action within cells called the MEK/ERK pathway. It's one of a class of drugs known as MEK inhibitors.
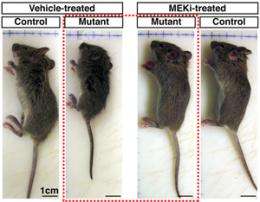
Mice with the NF1 mutation that got the drug from birth developed normally – in stark contrast to mice with the same genetic mutations that didn't receive the drug. The untreated mice appeared normal at birth, but within a few days had become hunched and scruffy, with abnormal growth of their bodies and brain cells.
The new paper's senior author, Yuan Zhu, Ph.D., cautions that the particular drug in the trial may not be appropriate to give to children who have been diagnosed with NF1. But other MEK inhibitors are being developed against cancer.
"The important thing is that we have shown that by treating during this brief window of time early in life, when neural stem cells in a developing brain still have time to 'decide' what kind of cell to become, we can cause a lasting effect on neural development," he says. Zhu is an associate professor of internal medicine, in the Division of Molecular Medicine and Genetics, and in the Department of Cell & Developmental Biology, at the Medical School.
The scientists didn't study the drug's effect on the behavior or learning ability of the mice, nor their tendency to develop benign brain tumors that can occur in NF1. In order for any such drug-based intervention to work most effectively, he notes, it would have to be given soon after developmental delays or benign tumors are noted in an infant or toddler, and after a NF1 diagnosis is made.
About half of all people with NF1 inherited the mutated gene from a parent, while about half developed it spontaneously in the womb. The disease affects individual patients very differently—one child born to a parent with mild NF1 can have a severe form of the disease, while their siblings can have mild or moderate symptoms.
Some people with NF1 have a "double hit" form of the disease, where both copies of the gene are mutated in certain body cells. The second mutation, the scientists say, likely occurs in a neural stem cell that goes on to produce unusual neural cells. These patients often have severe learning disabilities, and an enlarged corpus callosum—a structure that connects the two halves of the brain and contains a large concentration of glia, the same cells that the mice in the new study had larger numbers of.
In addition to NF1, the researchers predict that their findings may have importance for patients with other genetic conditions that affect the same general cell-signaling pathway called RAS. Collectively called neuro-cardio-facial-cutaneous (NCFC) syndromes or ''RASopathies", they include Leopard syndrome, Noonan syndrome, Costello syndrome and Leguis syndrome – all of which, like NF1, affect the brains, circulation system and the face or head.
The new research is based on several other discoveries made by current or former U-M faculty. The gene for NF1 was discovered in the late 1980s by Francis Collins, M.D., Ph.D. when he was a faculty member at the U-M Medical School, together with colleagues from other institutions. Collins is now director of the National Institutes of Health. That discovery paved the way for a genetic test that can now help definitively diagnose children with NF1, and guide their treatment.
Judith Sebolt Leopold, Ph.D., a research associate professor of radiology at the U-M Medical School, was a key member of the research team that developed PD0325901 while she worked at the Pfizer Research Laboratory formerly located in Ann Arbor.
The drug was first used in a cancer clinical trial in 2005, which was stopped when side effects on the retinas of some participants' eyes were noted. A new trial, using the drug in combination with another one, and comparing that combination with another drug combination, is now under way. Other MEK inhibitors, or MEKi drugs, are also in testing around the world, as scientists zero in on the RAS pathway as an important player in all kinds of cancer including melanoma.
More information: Cell, Volume 150, Issue 4, 816-830, 17 August 2012