Scientists have way to control sugars that lead to diabetes, obesity
(Medical Xpress)—Scientists can now turn on or off the enzymes responsible for processing starchy foods into sugars in the human digestive system, a finding they believe will allow them to better control those processes in people with type 2 diabetes and obesity.
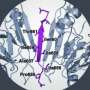
Bruce Hamaker, a professor of food science and director of the Whistler Center for Carbohydrate Research at Purdue University, said the four small intestine enzymes, called alpha-glucosidases, are responsible for generating glucose from starch digestion. Each enzyme functions differently, breaking down starches into different sugars at different rates. Someone missing one or more of those enzymes creates glucose improperly.
Influx of glucose to the blood increases insulin release from the pancreas, which allows the body to remove the sugar. When the body's tissues cannot respond well to insulin, the blood sugar is not lowered, a situation seen in type 2 diabetics. Even in non-diabetics, excess sugars not burned by the body as energy may be stored as fat, an issue for people prone to obesity.
"In diabetics, you don't want this roller coaster of blood-glucose levels. Their bodies can't regulate glucose that well," Hamaker said. "If you can selectively inhibit these enzymes, it opens up the possibility of moderating glucose to the body as well as directing glucose release into different parts of the small intestines for certain physiologic responses."
Hamaker and Mario Pinto, professor of chemistry and vice president for research at Simon Fraser University in Vancouver, Canada, members of a starch research consortium, led the study. Their results were published in the Journal of Biological Chemistry.
Hamaker's group did the inhibition studies on starch degradation products and the alpha-glucosidase enzymes, provided by other members of the consortium, in a simulated gastrointestinal tract system. The inhibitors, developed in Pinto's laboratory, were able to selectively inhibit the enzymes, a process they have called "toggling," and could lead to several solutions for diabetics or those prone to obesity.
"We could provide the missing enzymes or develop new starches that will digest properly with the enzymes they do have," Pinto said. "It's all about control and using the molecular information we have to control those enzymes."
Hamaker and Pinto said they would next work to understand how the inhibitors control the intestinal enzymes and refine their understanding of when and where the enzymes should be controlled for the best results.
More information: Modulation of Starch Digestion for Slow Glucose Release through 'Toggling' of Activities of Mucosal α-Glucosidases, Journal of Biological Chemistry.
ABSTRACT
Starch digestion involves the breakdown by α-amylase to small linear and branched malto-oligosaccharides, which are in turn hydrolyzed to glucose by the mucosal α-glucosidases, maltase-glucoamylase (MGAM) and sucrase-isomaltase (SI). MGAM and SI are anchored to the small intestinal brush-border epithelial cells, and each contains a catalytic N- and C-terminal subunit. All four subunits have α-1,4-exohydrolytic glucosidase activity, and the SI N-terminal subunit has an additional exo-debranching activity on the α-1,6-linkage. Inhibition of α-amylase and/or α-glucosidases is a strategy for treatment of type 2 diabetes. We illustrate here the concept of "toggling": differential inhibition of subunits to examine more refined control of glucogenesis of the α-amylolyzed starch malto-oligosaccharides with the aim of slow glucose delivery. Recombinant MGAM and SI subunits were individually assayed with α-amylolyzed waxy corn starch, consisting mainly of maltose, maltotriose and branched α-limit dextrins, as substrate in the presence of four different inhibitors: acarbose and three sulfonium ion compounds. The IC50 values show that the four α-glucosidase subunits could be differentially inhibited. The results support the prospect of controlling starch digestion rates to induce slow glucose release through the toggling of activities of the mucosal α-glucosidases by selective enzyme inhibition. This approach could also be used to probe associated metabolic diseases.