January 11, 2013 report
Researchers use hydrogel to repair cartilage
(Medical Xpress)—Researchers in the US have created a type of hydrogel that has proven to be effective in treating patients with damaged cartilage. The gel, the team writes, in their paper published in the journal Science Translational Medicine, thickens when exposed to light, providing a lattice platform for the development of new cell growth.
Cartilage is the pliable material that sits between bones that connect at the joints – its job is to serve as a buffer or cushion. Injuries to cartilage or simple wear and tear can result in perforations that allow bones to rub against one another causing difficulty in moving and pain. Sadly, cartilage doesn't generally repair itself the way other body parts do because it doesn't have a blood source. For that reason, doctors must intercede if a patient is to recover.
The traditional approach to repairing damaged cartilage is a procedure called microfracturing – doctors drill holes in the bone near the cartilage releasing blood and stem cells into the damaged area, promoting new cell growth. Unfortunately for such patients, the procedure doesn't fully restore cartilage to its former state and quite often leads to the formation of scar tissue. Because of this, many patients who experience cartilage damage, particularly in the knee, wind up with an artificial joint instead of repaired cartilage.
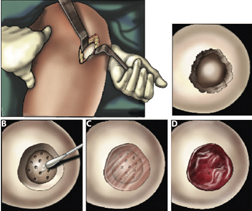
In this new approach, the researchers developed a hydrogel that when exposed to light, thickens into a Jell-O like substance with a crisscross lattice pattern. To make use of it, doctors first perform the standard microfracturing procedure. Once that's finished, they apply the gel to the holes in the cartilage, then finish by bathing it in light to cause it to thicken. The gel provides a platform for the stem cells to grow into cartilage cells, allowing for rejuvenation. Over time, the gel dissolves, leaving behind new cartilage.
To test how well the gel works, the team performed just the microfracturing procedure on one group of patients, and the combined procedure on another. They found that those that had received the gel had on average 86 percent closure of the perforations, whereas those that underwent just the microfracturing showed the normal 64 percent – a dramatic improvement, especially considering that those patients that received the gel also reported much less pain.
Because the number of patients in the study was small, more testing will have to be done to see just how effective the gel really is, of course. Thus far though, the results have been positive enough to suggest that the gel will likely become a standard treatment for cartilage repair in the very near future.
More information: Human Cartilage Repair with a Photoreactive Adhesive-Hydrogel Composite, Sci Transl Med 9 January 2013: Vol. 5, Issue 167, p. 167ra6 DOI: 10.1126/scitranslmed.3004838
ABSTRACT
Surgical options for cartilage resurfacing may be significantly improved by advances and application of biomaterials that direct tissue repair. A poly(ethylene glycol) diacrylate (PEGDA) hydrogel was designed to support cartilage matrix production, with easy surgical application. A model in vitro system demonstrated deposition of cartilage-specific extracellular matrix in the hydrogel biomaterial and stimulation of adjacent cartilage tissue development by mesenchymal stem cells. For translation to the joint environment, a chondroitin sulfate adhesive was applied to covalently bond and adhere the hydrogel to cartilage and bone tissue in articular defects. After preclinical testing in a caprine model, a pilot clinical study was initiated where the biomaterials system was combined with standard microfracture surgery in 15 patients with focal cartilage defects on the medial femoral condyle. Control patients were treated with microfracture alone. Magnetic resonance imaging showed that treated patients achieved significantly higher levels of tissue fill compared to controls. Magnetic resonance spin-spin relaxation times (T2) showed decreasing water content and increased tissue organization over time. Treated patients had less pain compared with controls, whereas knee function [International Knee Documentation Committee (IKDC)] scores increased to similar levels between the groups over the 6 months evaluated. No major adverse events were observed over the study period. With further clinical testing, this practical biomaterials strategy has the potential to improve the treatment of articular cartilage defects.
© 2013 Medical Xpress















