Hypersensitivity to pain produced by early life stress is worsened by later stress exposure
Childhood neglect and abuse, whether physical or psychological, confers a lifetime vulnerability to stress, anxiety, and mood problems. Such early-life stress is also suspected to contribute to the development of chronic pain in adulthood.
In fact, there is growing concern that chronic pain syndromes may be a complication of posttraumatic stress disorder (PTSD). However, this link is particularly challenging to study because many stressful events that produce PTSD also produce physical trauma. In addition, much of the research conducted in animals has not accurately reflected the early-life stress experienced by humans.
Inspired by a conversation with the violinist Itzhak Perlman, about students whose performance plateaued for unclear reasons, researchers led by Dr. Jon Levine at the University of California San Francisco, set out to rectify these gaps in understanding.
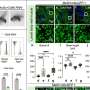
To do so, they used an animal model of maternal neglect that stresses rat mothers by restricting nesting/bedding material. These stressed rat mothers do not provide consistent levels of nurturing to their pups, i.e., the mothers are present but their care is unpredictable, resulting in increased levels of stress in the pups. The pups were otherwise not harmed or stressed.
Pups that had experienced this early-life stress showed increased reactivity to painful stimuli, particularly if they were exposed to a mild stress, an unpredictable unpleasant noise, as adults.
This enhanced muscle pain was related to both catecholamines, natural compounds in the body involved in the "fight-or-flight" response, and cytokines, molecules involved in the body's inflammatory response system. Interestingly, interventions that blocked the actions of the catecholamines and cytokines reduced the sensitivity to pain in the stressed pups.
"While it has been recognized for some time that early life events can shift homeostatic balance, predisposing adults to the development of chronic pain, that this could be mediated by a peripheral mechanism, involving the interaction between immune and neuroendocrine stress axes suggests novel approaches to detecting individuals at risk as well as to treatment of chronic pain," commented Levine.
This study suggests a 'two hit model' for the risk for pain syndromes: an initial stressor that predisposes to increased reactivity to later stress. The authors implicate both stress response and inflammation systems in the body in the link between stress and pain, potentially pointing to new treatment mechanisms.
"Chronic pain is a significant problem for people with PTSD. One reason for the co-occurrence of PTSD and pain is that the events that produce PTSD also may be associated with bodily harm. We have long known that childhood stress increases the vulnerability to PTSD. This new study also raises the possibility that early life stressors may increase the risk for pain syndromes," noted John H. Krystal, M.D., Editor of Biological Psychiatry.
More information: The article is "Stress in the Adult Rat Exacerbates Muscle Pain Induced by Early-Life Stress" by Pedro Alvarez, Paul G. Green, and Jon D. Levine (DOI: 10.1016/j.biopsych.2013.04.006 ). The article appears in Biological Psychiatry, Volume 74, Issue 9 (November 1, 2013)