Optimal site for cell transplantation to treat spinal cord injury investigated
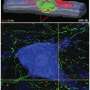
After laboratory mice received a contusive spinal cord injury at the T10 level, low and high doses of neural stem/progenitor cells (NS/PCs) derived from fetal bioluminescent-labeled transgenic mice were injected into four groups of mice at either the lesion epicenter or at rostral and caudal sites. A control group was similarly injected with phosphate buffered saline. The mice receiving the NS/PC cells experienced motor functional recovery while those in the control group did not.
It is known that transplanting neural stem/progenitor cells (NS/PCs) into the spinal cord promotes functional recovery after spinal cord injury (SCI). However, which transplantation sites provide optimal benefit? This question was investigated by a Japanese research team and their findings will be published in a future issue of Cell Transplantation, but are currently freely available on-line as an unedited early e-pub.
"It is critical to determine the optimal transplantation site for NS/PCs aimed at treating SCI," said Dr. Masaya Nakamura of the Department of Orthopedic Surgery at the Keio University School of Medicine.
Previous work by the same research team revealed that NS/PCs injected into non-injury sites such as by intravenous or intrathecal administration did not engraft to the injury site in sufficient numbers, but instead were often "trapped" in the lungs and kidneys. They concluded that intralesional application might be the most effective and reliable method for transplanting NS/PCs. This study, also using laboratory mice with SCI, sought to determine how effective intralesional injection might be. NS/PCs were obtained from mice transgenic for Venus and luciferase fusion protein, which allowed the cells to be tracked by bioluminescence imaging (BLI) after transplantation.
"Wild-type mice were given a contusive spinal cord injury at the T10 level," explained Dr. Nakamura. "Low and high doses of NS/PCs derived from fetal transgenic mice were injected into four groups of mice at either the lesion epicenter (E) or at rostral and caudal sites (RC) with neural stem/progenitor cells derived from fetal transgenic mice while a fifth group of controls was injected with phosphate buffered saline at E."
According to the researchers, all four groups of mice receiving the cells experienced motor functional recovery while those in the control group did not. They also found that the photon counts from BLI of the grafted NS/PCs were similar in each of the four transplantation groups.
"This suggests that the survival of the NS/PCs was fairly uniform when more than a certain threshold number of cells were transplanted," said the researchers. "However, analysis showed that brain-derived neurotropic factor expression was higher in the RC segment than in the E segment."
This result may explain why transplanted NS/PCs appeared to differentiate more readily into neurons than astrocytes in the RC group due to the impact of the enhanced expression of the brain-derived neurotrophic factor.
"This may mean that the microenvironments of the E and RC sites are similarly able to support NS/PCs transplanted during the sub-acute phase of SCI," they concluded.
"This study provides evidence that the lesion microenvironment can support cell survival" said Dr. John Sladek, Cell Transplantation section editor and professor of neurology and pediatrics at the University of Colorado School of Medicine "The next step is to determine the factors that will impact favorably on the optimization of the cell transplantation site."
More information: Iwai, H.; Nori, S.; Nishimura, S.; Yasuda, A.; Takano, M.; Tsuji, O.; Fujiyoshi, K.; Toyama, Y.; Okano, H.; Nakamura, M. Transplantation of neural stem/progenitor cells at different locations in mice with spinal cord injury. Cell Transplant. Appeared or available online: August 30, 2013