Brainy biomechanics for safer brain surgery
(Medical Xpress)—Patients undergoing brain surgery are likely to benefit from a new technique that can help neurosurgeons predict how the brain will move during operations.
The technique was developed by researchers at The University of Western Australia and colleagues at Harvard Medical School in the US. Their article describing the breakthrough was recently accepted by the Journal of Neurosurgery.
Winthrop Professor Karol Miller, Deputy Head of UWA's School of Mechanical and Chemical Engineering and Director of the University's Intelligent Systems for Medicine Laboratory, is the team leader. He has been working in this field for nine years and is well-known internationally for his work on neuro-navigation. He is also Honorary Distinguished Professor of Engineering at Cardiff University in the UK.
Professor Miller said there is a fine line for surgeons between taking enough of a brain tumour out and leaving too much behind - and the work carried out in his lab and at Harvard is set to revolutionise this surgery, to make the procedure easier and to improve patient outcomes.
Professor Miller explained it was essential for surgeons to know exactly how a soft organ, such as the brain, would change shape, or 'deform', during surgery. A pre-surgery magnetic resonance image (MRI) gives an accurate picture of the brain and the location of the tumour before the start of the operation, but during the operation the organ changes significantly and crucially, due to factors including anaesthesia, cerebrospinal fluid flow and interactions with surgical instruments.
"Traditionally, surgeons use 'mental projection' to estimate these changes, which can be up to 20 mm," he said. "Our work provides a patient-specific, very cost effective, very fast, very sophisticated intra-operatic guide that surgeons use while they are operating. Thanks to our algorithms working perfectly on graphics processing units, within 10 seconds one can get an accurate picture of the complexity of deformations from a basic computer.
"This means that neurosurgeons are more likely to feel confident cutting more of the tumour out, knowing they are leaving the healthy tissue behind," he said.
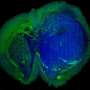
Professor Miller and his team use digitised models of a patient's brain that are developed from MRI. By segmenting 3D magnetic resonance volumes the neuro-images are transformed into geometric meshes or computational grids. They show, in different colours, the tumour, healthy tissue, and ventricles.
The images are then used for real-time computer simulation of the brain's deformation during surgery. The results can be viewed from every angle during the operation. The technology is so fast and easy to use that it does not interfere with a traditional operating surgery schedule.
Professor Miller said the technique provided better data, particularly for patients with large brain shift.