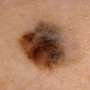
Long-term study confirms success of method for detecting spread of deadly skin cancer
Research at UCLA on a technique for detecting the earliest spread of melanoma, the deadliest form of skin cancer, has confirmed that the procedure significantly prolongs patients' survival rates compared with traditional "watch and wait" techniques.
The technique, which combines lymphatic mapping and sentinel-node biopsy, allows doctors to quickly determine whether the disease has spread, or metastasized, to the lymph nodes, which occurs in approximately 20 percent of patients. Patients with cancer in their lymph nodes may benefit from having their other nearby lymph nodes removed. For the other approximately 80 percent of patients in whom the tumors have not spread to the lymph nodes, the technique spares the patient from unnecessary surgery and its associated complications and substantial costs.
The results of the decade-long study, which began at UCLA's Jonsson Comprehensive Cancer Center, were published Feb. 13 in the New England Journal of Medicine. The research was led by Dr. Donald Morton, UCLA professor emeritus of surgery and director of the John Wayne Cancer Institute in Santa Monica, and Dr. Alistair Cochran, professor in the department of surgery and the department of pathology and laboratory medicine at the David Geffen School of Medicine at UCLA. Morton died in January at the age of 79.
Researchers evaluated outcomes of 2,001 melanoma patients after 10 years. The results confirmed that lymphatic mapping and sentinel-node biopsy have been a significant advance in the treatment of melanoma—the method improved patients' long-term melanoma-specific survival and their survival without cancer spreading to other parts of the body.
"Long-term follow-up shows a survival advantage with our technique, a finding that was only detectable with a 10-year analysis," Cochran said. "This is very gratifying for all who worked on developing and testing the approach at UCLA and in centers around the world."
One important finding was that the thickness of the initial melanoma tumor determined the effectiveness of the treatments in managing nodal and other metastases. Patients who had primary melanoma tumors of intermediate thickness (1.2 to 3.5 millimeters thick) and whose lymph nodes were completely removed after a positive biopsy had a disease-free survival rate of 71.3 percent after 10 years, compared with a 64.7 percent rate for those whose nodes were observed without sentinel biopsy.
The study confirmed that for patients with intermediate-thickness melanomas, early sentinel biopsy decreases the risk of cancer recurring in the lymph nodes and decreases their chances of dying from melanoma.
The research also found that sentinel-node biopsy prolonged the patients' survival without melanoma spreading to the brain, lungs, liver or other organs; and that it improved the survival rate for patients with lymph node metastasis from primary melanomas of intermediate thickness without additional metastases.
In 20 percent of patients with melanoma, the cancer has already spread to nearby lymph nodes when they are diagnosed with the disease. Traditionally, these patients underwent surgery to remove the primary tumor and a rim of normal tissue around it, followed by clinical observation of the lymph nodes throughout their follow-up care, or until the disease was detected in the lymph nodes. If the lymph nodes developed signs of cancer over time, they were surgically removed.
Although the observation method spared 80 percent of patients from unnecessary surgery and its considerable risk of complications, the detection of metastases in the lymph nodes may have occurred too late to stop the spread of the disease.
The primary alternative to the observation method was to remove all patients' lymph nodes, since every patient was potentially at risk of metastasis; but this option subjected 80 percent of patients to unnecessary surgery. That prompted Morton, Cochran and their colleagues in the UCLA division of surgical oncology to develop the sentinel-node biopsy method for identifying the 20 percent of patients whose tumors had already spread to the lymph nodes. The first results from their phase 3 trial comparing their method with standard observation were published in 2001.
Before cancer cells spread throughout the lymph nodes, they travel through the lymphatic vessels, first entering the sentinel lymph node, which is the lymph node most directly connected to the primary tumor. In the technique developed at UCLA, doctors inject the tissue near the primary tumor with a mixture of blue dye and radioactive tracer to find the lymphatic channels that lead directly to the tumor-draining sentinel lymph node. The dye–isotope mixture follows the same lymphatic path as the melanoma cells that spread to the sentinel node. Doctors can then remove the sentinel node and examine it in detail under a microscope using probes that are sensitive enough to detect even single melanoma cells.
If melanoma cells are not found in the sentinel node, it is highly unlikely that there will be tumors in other non-sentinel nodes, meaning that further nodal surgery is not necessary. If melanoma cells are present, however, doctors typically decide immediately to remove all other lymph nodes of the nodal group. The technique has become widely used and is now viewed as a practice-changing development.
Although some patients with thick primary tumors (thicker than 3.5 millimeters) benefit from having their lymph nodes removed, the trial data suggest that the timing of the intervention is not as crucial for them as it is for patients with intermediate thickness primary tumors. The trial did not evaluate enough patients with thin melanomas (less than 1.20 millimeters thick) to understand how they might benefit from lymphatic mapping and sentinel-node biopsy.