Personalized melanoma vaccines marshal powerful immune response
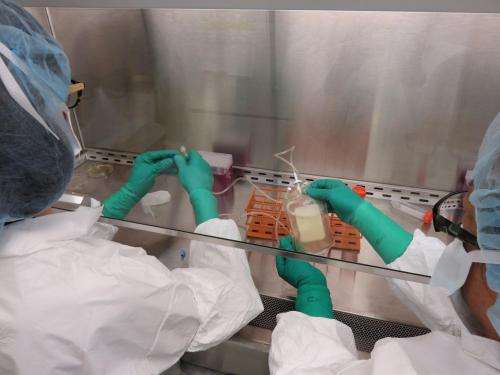
Personalized melanoma vaccines can be used to marshal a powerful immune response against unique mutations in patients' tumors, according to early data in a first-in-people clinical trial at Washington University School of Medicine in St. Louis.
The tailor-made vaccines, given to three patients with advanced melanoma, appeared to increase the number and diversity of cancer-fighting T cells responding to the tumors. The finding is a boost to cancer immunotherapy, a treatment strategy that unleashes the immune system to seek out and destroy cancer.
The research is reported April 2 in Science Express, in a special issue devoted to cancer immunology and immunotherapy.
In a new approach, the cancer vaccines were developed by first sequencing the genomes of patients' tumors and samples of the patients' healthy tissues to identify mutated proteins called neoantigens unique to the tumor cells. Then, using computer algorithms and laboratory tests, the researchers were able to predict and test which of those neoantigens would be most likely to provoke a potent immune response and would be useful to include in a vaccine.
The vaccines were given to melanoma patients who had had surgery to remove their tumors but whose cancer cells had spread to the lymph nodes, an indicator the deadly skin cancer is likely to recur. These clinical findings set the stage for a phase I vaccine trial, approved by the Food and Drug Administration as part of an investigational new drug application. The trial will enroll six patients.
Data on the immune response seen in the first three patients is reported in the paper. If additional testing in more patients indicates the vaccines are effective, they may one day be given to patients after surgery to stimulate the immune system to attack lingering cancer cells and prevent a recurrence.
"This proof-of-principle study shows that these custom-designed vaccines can elicit a very strong immune response," said senior author Gerald Linette, MD, PhD, a Washington University medical oncologist leading the clinical trial at Siteman Cancer Center and Barnes-Jewish Hospital. "The tumor antigens we inserted into the vaccines provoked a broad response among the immune system's killer T cells responsible for destroying tumors. Our results are preliminary, but we think the vaccines have therapeutic potential based on the breadth and remarkable diversity of the T-cell response."
It's too early to say whether the vaccines will be effective in the long term, the researchers cautioned. The study was designed to evaluate safety and immune response; however, none of the patients has experienced adverse side effects.
Earlier attempts at vaccines have focused on targeting normal proteins commonly expressed at high levels in particular cancers. Those same proteins also are found in healthy cells, making it difficult to stimulate a potent immune response.
The new approach investigated by the Washington University team merges cancer genomics with cancer immunotherapy.
"This is about as personalized as vaccines can get," said co-author Elaine Mardis, PhD, co-director of the McDonnell Genome Institute at Washington University, where the cancer genome sequencing, analysis and neoantigen prediction were performed. "The approach we describe is fundamentally different from conventional mutation discovery, which focuses on identifying mutated genes that drive cancer development. Instead, we're looking for a unique set of mutated proteins in a patient's tumor that would be most likely to be recognized by the immune system as foreign."
Melanomas are notorious for having high numbers of genetic mutations caused by exposure to ultraviolet light. Biopsy samples of melanomas typically carry 500 or more mutated genes. Using prediction algorithms, the researchers narrowed their search for vaccine candidates by identifying neoantigens that not only were expressed in a patient's tumor but also were likely to be seen by that patient's immune system as "non-self."
Biochemical validation of neoantigen peptide expression on the cancer cells' surfaces was performed in collaboration with William Hildebrand's group at the University of Oklahoma Health Sciences Center and provided critical assurance that the vaccine would elicit the most effective T cells to combat the melanoma.
"You can think of a neoantigen as a flag on each cancer cell," said first author Beatriz Carreno, PhD, associate professor of medicine. "Each patient's melanoma can have hundreds of different flags. As part of validating candidate vaccine neoantigens, we were able to identify the flags on the patients' cancer cells. Then we created customized vaccines to a select group of flags on each patient's tumor."
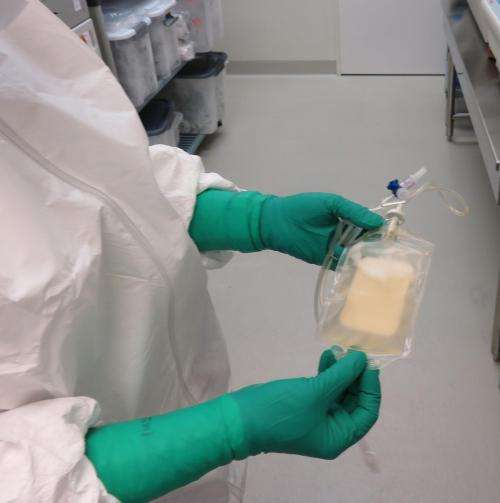
Carreno and her colleagues selected a set of seven unique neoantigens for each vaccine and used specialized immune cells called dendritic cells, derived from the patients, to carry those neoantigens to the immune system. Dendritic cells play an important role in waking up the immune system, reminding T cells to attack the cancer.
After the vaccine infusions, the patients' blood was drawn every week for about four months. By analyzing the blood samples, the researchers could see that each patient mounted an immune response to specific neoantigens in their vaccines. The vaccines also stimulated diverse clones of battle-ready T cells against neoantigens, suggesting this approach also could be used to activate a range of T cells and target them to mutations in other cancers with high mutation rates, such as lung cancer, bladder cancer and certain colorectal cancers.
"Our team has developed a new strategy for personalized cancer immunotherapy," Linette said. "Many researchers have hypothesized that it would be possible to use neoantigens to broadly activate the human immune system, but we didn't know that for sure until now. We still have much more work to do, but this is an important first step and opens the door to personalized immune-based cancer treatments."
More information: A dendritic cell vaccine increases the breadth and diversity of melanoma neoantigen-specific T cells, www.sciencemag.org/lookup/doi/ … 1126/science.aaa3828