Mechanism identified for enhancing immunological memory in helper T cells
Vaccines help prevent disease by inducing immunological memory, the ability of immune cells to remember and respond more quickly when re-exposed to the same pathogen. While certain phases of the pathway are well understood, little is known about the role of helper T cells, a "master orchestrator" of the immune response that send signals to activate the immune system.
A study led by the University of Utah School of Medicine has identified molecular mechanisms that control an immune cell's ability to remember. They found that in helper T (CD4+) cells, the proteins Oct1 and OCA-B work together to put immune response genes on standby so that they are easily activated when the body is re-exposed to a pathogen. The research, which could inform strategies for developing better vaccines, was performed in collaboration with scientists from The Broad Institute and University of Michigan, and published in The Journal of Experimental Medicine.
For immunological memory to be effective, genes that are turned off in immune cells following an infection have to be rapidly turned back on when the body reencounters a pathogen. Previous work in the lab of Dean Tantin, Ph.D., senior author and associate professor in pathology at the University of Utah, showed that the transcription factor Oct1 is required for 'poising' Il2, a gene important for immunity, in a state where it can be activated quickly if needed.
"Oct1 is unusual in that it often times doesn't activate a gene or repress a gene," explained Tantin. "It can act as an insulator to prevent genes from getting permanently turned off."
They showed that Oct1 blocks stable repression of genes involved in immunity in resting cells that had been previously activated by a pathogen. Oct1 removed epigenetic tags that ordinarily ensure that Il2 stays turned off. However, Tantin noted that the signaling cues used by Oct1 in activated cells were missing in resting memory T cells that had previously been activated, indicating that there must be another factor needed for Il2 expression.
In this study, Shakya et al. identified OCA-B as being the additional factor required for a robust immune response in resting helper T cells. OCA-B was expressed in activated and re-activated helper T cells and was required, together with Oct1, for removal of repressive epigenetic marks from the Il2 gene. Also, helper T cells from OCA-B deficient mice did not produce as much IL-2 as normal cells when stimulated in culture. The findings demonstrate that OCA-B is required for the activation of Il2, and they present evidence that it additionally regulates a group of 50 - 100 genes in re-stimulated cells.
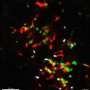
To further investigate the importance of Oct1 and OCA-B in immunological memory, the researchers examined mice lacking either one of the two genes. Months after infection with a pathogenic virus, OCA-B or Oct1 deficient animals had fewer memory T cells compared to control animals. After reinfection with the same virus, memory cells in the Oct1 and OCA-B deficient animals failed to generate a recall response.
These findings show that Oct1 and OCA-B are involved in memory T cell function and are necessary for the helper cell memory response. Results from this research add to the understanding of how a memory response is generated, which could potentially have therapeutic applications.
"If you had pharmaceutics that could augment this process, you potentially could make better vaccines," said Tantin. "If you interfered with it, you could inhibit memory formation or function, which might be a valid therapeutic for autoimmunity." Future studies in his lab will pursue these therapeutic possibilities.
More information: "Oct1 and OCA-B are selectively required for CD4 memory T cell function" was published in The Journal of Experimental Medicine online on October 19, 2015