Cellular immunotherapy targets a common human cancer mutation
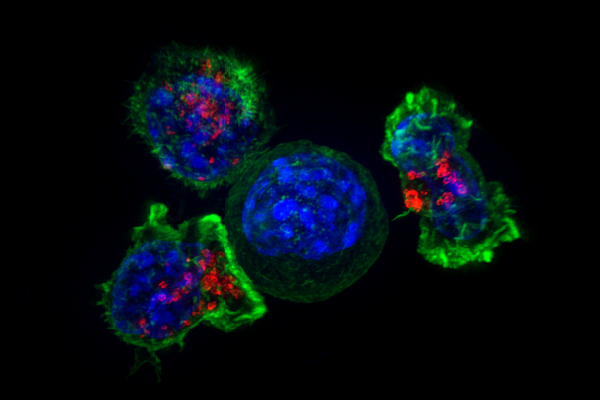
In a study of an immune therapy for colorectal cancer that involved a single patient, a team of researchers at the National Cancer Institute (NCI) identified a method for targeting the cancer-causing protein produced by a mutant form of the KRAS gene. This targeted immunotherapy led to cancer regression in the patient in the study. The finding appeared Dec. 8, 2016, in the New England Journal of Medicine. The study was led by Steven A. Rosenberg, M.D., Ph.D., chief of the Surgery Branch at NCI's Center for Cancer Research, and was conducted at the NIH Clinical Center. NCI is part of the National Institutes of Health.
More than 30 percent of all human cancers are driven by mutations in a family of genes known collectively as RAS, which has three members: KRAS, NRAS, and HRAS. Mutations in the KRAS gene are thought to drive 95 percent of all pancreatic cancers and 45 percent of all colorectal cancers. A mutation called G12D is the most common KRAS mutation and is estimated to occur in more than 50,000 new cases of cancer in the United States each year. Because of their importance in cancer causation, worldwide efforts to successfully target mutant RAS genes are being pursued. Such efforts have met with limited success to date.
In attempting to develop more effective approaches to targeting RAS, Rosenberg's team isolated tumor infiltrating lymphocytes (TILs) that targeted the KRAS G12D mutation from tumor nodules in the patient's lungs that developed after colorectal cancer cells had spread to the lungs. TILs are white blood cells that migrate from the bloodstream into a tumor.
The isolated TILs were grown in the laboratory to large numbers and then infused into the patient intravenously. Following the TIL infusion, all seven metastatic lung nodules in the patient regressed, and the regression persisted for nine months.
After nine months, one of the lesions progressed and was surgically removed. This lesion was found to have lost a segment of chromosome 6 that includes a gene known as HLA-C*0802. This gene is involved in antigen presentation, a process through which an antigen produced by a cell is displayed on the cell's outer surface and is thereby "presented" to the immune system. If the immune system recognizes the antigen as abnormal or foreign, an immune response against it will be mounted. In this case, because of the loss of the segment of chromosome 6, the immune system was unable to recognize the cancer cells as being abnormal, and they were able to escape immune attack and continue to thrive. Since the lesion was removed, however, the patient has been disease-free for over eight months.
"This study demonstrates for the first time, that this method of administering TILs, called adoptive T cell transfer immunotherapy, can mediate effective antitumor immune responses against cancers that express the KRAS G12D mutation," said Dr. Rosenberg. "We have also identified multiple T cell receptors that recognize this KRAS product, thus opening the possibility of T cell receptor gene therapy against multiple types of cancer that express this common mutation."
The authors of the study note that this work is a proof-of-principle and that the next step is to see if the method proves effective in other patients.
More information: Tran E, Rosenberg SA, et al. T-cell transfer therapy targeting mutant KRAS in cancer. December 8, 2016. NEJM. DOI: 10.1056/NEJMoa1609279