Aging-related mutations in blood cells represent major new risk factor for cardiovascular disease

Scientists at the Broad Institute of MIT and Harvard have found that a set of genetic mutations in blood cells that arises during aging may be a major new risk factor for cardiovascular disease. In contrast to inherited genetic predispositions and traditional lifestyle risk factors, such as smoking or an unhealthy diet, the new mutations are "somatic mutations" that originate in stem cells in the bone marrow as people age.
Because the mutations are relatively common in older people (over 10% of people over the age of 70 harbor at least one of these mutations), potential future efforts to screen for the mutations in blood cells, identify people at increased risk for coronary heart disease, and reduce risk in those individuals through lifestyle changes or therapeutic interventions could have a significant clinical impact, according to the researchers.
"There is more work to be done, but these results demonstrate that pre-malignant mutations in blood cells are a major cause of cardiovascular disease that in the future may be treatable either with standard therapies or new therapeutic strategies based on these findings," said Benjamin Ebert, a co-senior author of the new study, an institute member at the Broad, a professor of medicine at Harvard Medical School, and a hematologist at Brigham and Women's Hospital.
Featured in the New England Journal of Medicine, the work also contributes to the broader understanding of pathogenesis in coronary heart disease by supporting the hypothesis that inflammation, in addition to elevated cholesterol levels, plays an important role in this illness and potentially other diseases of aging.
"A key finding from this study is that somatic mutations are actually modulating risk for a common disease, something we haven't seen other than in cancer," said first author Siddhartha Jaiswal, a pathologist at Massachusetts General Hospital and researcher in the Ebert lab. "It opens up interesting questions about other diseases of aging in which acquired mutations, in addition to lifestyle and inherited factors, could modulate disease risk."
Previous research led by Ebert and Jaiswal revealed that some somatic mutations that are able to confer a selective advantage to blood stem cells become much more frequent with aging. They named this condition "clonal hematopoiesis of indeterminate potential," (CHIP), and found that it increases the risk of developing a blood cancer more than 10-fold and it appeared to increase mortality from heart attacks or stroke. In the new study, the researchers analyzed data from four case-control studies on more than 8,000 people and found that having one of the CHIP-related mutations nearly doubled the risk for coronary heart disease, with the mutations conferring an even greater risk in people who have previously had a heart attack before age 50.
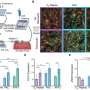
While the human genetics data showed a strong association between CHIP and coronary heart disease, the team hoped to uncover the underlying biology. Using a mouse model prone to developing atherosclerosis, the scientists showed that loss of one of the CHIP-mutated genes, Tet2, in bone marrow cells leads to larger atherosclerotic plaques in blood vessels, evidence that this mutation can accelerate atherosclerosis in mice.
Atherosclerosis is believed to be a disease of chronic inflammation that can arise in response to excess cholesterol in the vessel wall. To examine this on a cellular level the team turned to the macrophage, an immune cell found in atherosclerotic plaques that can develop from CHIP stem cells and carry the same mutations. Because Tet2 and other CHIP-related mutations are known to be so-called "epigenetic regulators" that can alter the activity of other genes, the team examined gene expression levels in the Tet2-mutated macrophages from mice. They found that the mutated cells appear to be "hyper-inflammatory" with increased expression of inflammatory molecules that contribute to atherosclerosis. In support of this finding, humans with TET2 mutations also had higher levels of one of these molecules, IL-8, in their blood.
The work demonstrates that CHIP associates with coronary heart disease in humans, that mutation of the CHIP-related gene Tet2 causes atherosclerosis in mice, and that an inflammatory mechanism likely underlies the process. More work is needed to show whether other genes that are mutated in CHIP also lead to increased inflammation. The team is also exploring whether interventions such as cholesterol lowering therapy or anti-inflammatory drugs might have benefit in people with CHIP.
Inflammation is also thought to modulate several other diseases of aging besides cardiovascular disease, such as autoimmune disorders and neurodegenerative disease. Because CHIP also increases in frequency with age, somatic mutations that alter inflammatory processes could influence several diseases of aging, though more work is needed to test this possibility.
"By combining genetic analysis on large cohorts with disease model and gene expression studies, we've been able to confirm the earlier hints of CHIP's surprising role in cardiovascular disease," said co-senior author Sekar Kathiresan, director of the Broad's Cardiovascular Disease Initiative, associate professor of medicine at Harvard Medical School, and director of the Center for Genomic Medicine at Massachusetts General Hospital. "Beyond the mutations that you inherit from your parents, this work reveals a new genetic mechanism for atherosclerosis—mutations in blood stem cells that arise with aging."
More information: Siddhartha Jaiswal et al. Clonal Hematopoiesis and Risk of Atherosclerotic Cardiovascular Disease, New England Journal of Medicine (2017). DOI: 10.1056/NEJMoa1701719