Personalized diagnostic assay for the treatment of knee injuries
An article published in Experimental Biology and Medicine (Volume 242, Issue 18, December 2017) describes a new approach for profiling patients with joint injuries. The study, led by Dr. Ursula Anderer, Professor for Cell Biology and Head of the Department Cell Biology and Tissue Engineering at Brandenburg University of Technology in Cottbus-Senftenberg, Germany, demonstrates that a microtissue culture assay can be used to identify patients that will benefit from cell-based therapies.
Trauma- and osteoarthritis-related joint injuries are rising due to increases in life expectancy and the number of individuals participating in sports-related activities. A central event in joint injuries is damage to or loss of cartilage, the strong elastic tissue in joints that absorbs shock and allows bones to smoothly glide past each other. Because the ability of cartilage to self-repair is limited, treatment options include replacing the damaged tissue with artificial cartilage or transplanting cells, chondrocytes, that can generate new cartilage. While using a patient's own cells (autologous transplantation) has the fewest side effects, this approach does not always produce functional cartilage. A personalized diagnostic tool that can predict the ability of a patient's cells to form functional cartilage would improve outcomes for patients with joint injuries.
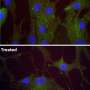
In the current study, Dr. Anderer and colleagues used a three-dimensional (3-D) cell culture technique to assess the ability of cartilage cells isolated from human donors to form cartilage. Previous studies have demonstrated that chondrocytes grown as a monolayer using standard two-dimensional (2-D) cell culture techniques do not retain the characteristics associated with mature chondrocytes. In contrast, chondrocytes grown in a more physiological 3-D environment that promotes organization into a tissue, resemble mature chondrocytes.
All of the donor cells examined in this study exhibited an identical chondrocyte profile in 2-D culture. However, there were clear differences in chondrogenic potential among individual donors in 3-D microtissues. These findings suggest that this 3-D assay may be a suitable personalized diagnostic tool for identifying patients that will benefit from autologous cell-based therapy.
Dr. Anderer said, "Choosing a cell culture system which is as close as possible to the natural tissue situation made it possible to identify personalized tissue forming properties in vitro. This individualized characterization of the potency of cartilage cells will be the basis for a patient profile by identification of specific intrinsic markers (biomarkers) to classify these patients."
Dr. Steven R. Goodman, Editor-in-Chief of Experimental Biology & Medicine, said, "Anderer and colleagues have provided a 3-D microtissue in vitro model platform that they demonstrate to be of value in predicting the personalized therapeutic value of autologous cell-based cartilage repair. This could be a valuable step towards regenerative medicine for traumatic or degenerative defects of cartilage tissue."
More information: Frank Martin et al. Featured Article: In vitro development of personalized cartilage microtissues uncovers an individualized differentiation capacity of human chondrocytes, Experimental Biology and Medicine (2017). DOI: 10.1177/1535370217728498