Leukemia-causing retrovirus HTLV-1 vaccine a future possibility
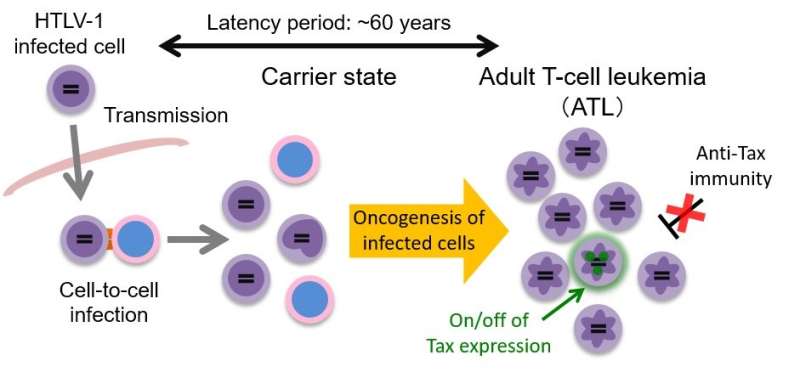
A study appearing in the in Proceedings of the National Academy of Sciences gives new clues into how cancers like leukemia form from the retrovirus HTLV-1, as well as insights into the possible creation of a vaccine.
HTLV-1 is a human retrovirus that mainly infects the CD4+ T cell. Such Infections can lead to a host of immune-related diseases including leukemia. Somewhat counterintuitively, the virus thrives by remaining at very low levels in the body, which is unlike its more notorious cousin, HIV.
"HTLV-1 RNA is rarely detected in the plasma of infected individuals, and it persists by evading host immune surveillance," says Jun-ichirou Yasunaga of Kyoto University's Institute for Frontier Life and Medical Sciences, who led the study.
HTLV-1 encodes two oncogenic factors, Tax and HBZ. Besides its function as an oncoprotein, Tax also facilitates viral replication. "The precise role of Tax in pathogenesis is unknown, since it is so faintly expressed in infected cells," continues Yasunaga.
The researchers found that within populations of infected leukemic cells, only a tiny fraction—less than 3 percent—expressed Tax. Moreover, this expression in any given cell was transient, lasting less than 24 hours. However, while the cells that expressed Tax would change over time, more than 3 percent of the population would express this gene.
In fact, in vitro experiments showed that if Tax expression was suppressed in this small population, then almost all infected cells would vanish in less than a month. Furthermore, computational simulations found that it takes about five months for 90 percent of the infected cells to express Tax. This transience is advantageous for the survival of the virus, since persistent Tax expression is associated with an immune response.
Yasunaga explains that keeping the expression of Tax limited to a small population allows the infection to flourish and prevent the infected cells from undergoing controlled death, known as apoptosis. "There were clear differences in the gene expression between Tax-expressing and Tax-non-expressing cells. In the latter, there were two populations, those with medium, and those with low levels of anti-apoptotic factors. This shows that Tax caused different degrees of sensitivity to apoptosis," he explains.
Further studies revealed that this effect on apoptosis sensitivity was found in cells with better overall survivability. Yasunaga hypothesizes that even if cells stop expressing Tax, those with medium levels of anti-apoptosis factors are more resistant to apoptosis, allowing these cells to survive.
"Transient Tax expression enhances the survival and proliferation of infected cells, so it's a good vaccine target. Understanding its expression mechanism could be a key to new therapies," says Yasunaga.
More information: Mohamed Mahgoub et al, Sporadic on/off switching of HTLV-1 Tax expression is crucial to maintain the whole population of virus-induced leukemic cells, Proceedings of the National Academy of Sciences (2018). DOI: 10.1073/pnas.1715724115