Researchers uncover potential new drug targets in the fight against HIV
Johns Hopkins scientists report they have identified two potential new drug targets for the treatment of HIV. The finding is from results of a small, preliminary study of 19 people infected with both HIV—the virus that causes AIDS—and the hepatitis C virus. The study revealed that two genes—CMPK2 and BCLG, are selectively activated in the presence of type 1 interferon, a drug once used as the first line of treatment against hepatitis C.
Results of the study were published online Aug. 1 in Science Advances.
"We've known that HIV worsens our ability to treat hepatitis C with type 1 interferon, but why that was has been unclear. In some way the viruses' interactions with each other and with the treatment seemed at the root of the failure," says Ashwin Balagopal, M.D., associate professor of medicine at the Johns Hopkins University School of Medicine.
To study the relationship, the researchers enrolled 19 participants—15 men and four women, all over the age of 20—from several Baltimore clinics, including the Johns Hopkins HIV Clinic and a Baltimore City Health Department sexually transmitted disease clinic. All participants were diagnosed with chronic HIV and hepatitis C infections.
The participants received injections of interferon to treat their hepatitis C. Before and after each treatment, the researchers took blood samples to measure the amount of both hepatitis C and HIV present in the blood.
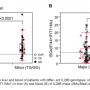
After one week of treatment, the participants had on average 10 times less HIV in their blood.
"This told us that the interferon we were using to treat hepatitis C was working to control HIV as well, but we needed to investigate how it was accomplishing this," says Balagopal.
To do this, Balagopal and his colleagues studied the patients' CD4 T cells—the immune cells most suppressed and affected by HIV—in the lab.
In those cells, the researchers measured the levels of numerous gene products before and after interferon treatment.
They identified 99 genes with higher levels of expression after interferon treatment. Of these genes, the researchers found that two, CMPK2 and BCLG, had not been previously linked to HIV. Both genes are thought to be involved in the processes that guide how cells divide.
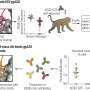
The researchers then infected lab-grown human cells (not from the 19 patients) with HIV to further study the interactions between the two genes and interferon.
First, they engineered human immune cells to render them unable to produce the protein made by the CMPK2 gene. They then added interferon and tested the cells' HIV levels, finding that control cells with functioning CMPK2 had 10 times less HIV than cells in which CMPK2 was blocked.
On the other hand, BCLG normally has very low expression levels, according to the investigators, and is difficult to eliminate from human cells. So the researchers opted to increase its expression by adding more BCLG genes to HeLa cells infected with HIV in the lab.
The researchers then again added interferon to the cells and 48 hours later, the cells engineered to have more BCLG expression had half the amount of HIV compared to cells with normal BCLG expression.
This seems to indicate that CMPK2 and BCLG play a role in interferon's ability to suppress HIV, according to Balagopal, and potentially could serve as targets for new drug approaches to HIV treatment, particularly in people who are co-infected.
The researchers caution that the level of HIV suppression they saw in these interferon experiments is not large enough to warrant interferon's use as a standalone treatment.
More than 1.1 million people in the U.S. are living with HIV and 25 percent of them are estimated to be co-infected with the hepatitis C virus. The researchers say nearly one-third of the HIV patients in their Baltimore clinics also have hepatitis C. Hepatitis C causes inflammation of the liver and, though it can take years for symptoms to arise, can cause nausea, weight loss, cirrhosis, liver cancer and liver failure. Complications from this virus are accelerated in people co-infected with HIV.
In the future, Balagopal hopes to better understand the genes and their roles in HIV suppression by investigating the cellular pathways with which they interact. He also hopes to examine the genes' effects on HIV's ability to hide for decades within cells—a factor that has stalled scientists' efforts to cure HIV infections.
More information: Ramy El-Diwany et al. CMPK2 and BCL-G are associated with type 1 interferon–induced HIV restriction in humans, Science Advances (2018). DOI: 10.1126/sciadv.aat0843