Study links obesity with pancreatitis
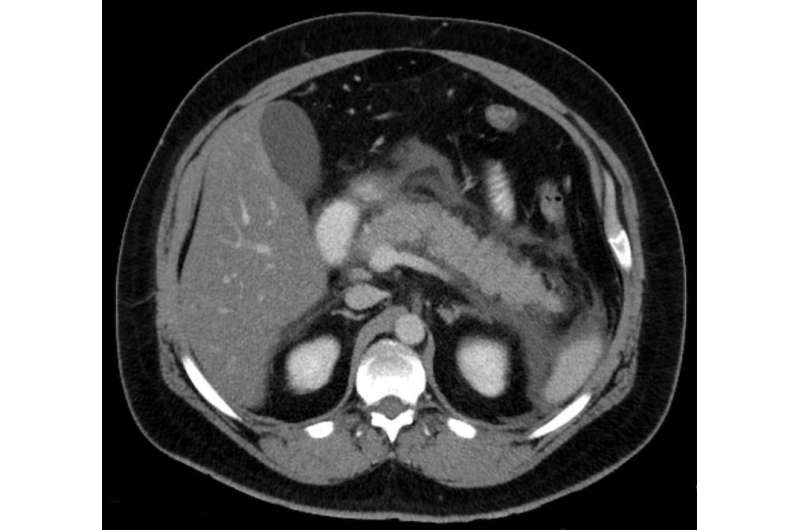
A study by researchers at Mayo Clinic in Arizona published in the the Journal of Clinical Investigation has found that obesity is not only implicated in chronic diseases such as diabetes, but also in sudden-onset diseases such as pancreatitis.
"In our study, we were able to demonstrate that fat within the belly is rapidly degraded during acute pancreatitis, but not during diverticulitis, despite inflammation," says Vijay Singh, M.B.B.S., a Mayo Clinic gastroenterologist. Dr. Singh says while both diseases present with sudden belly pain and account for about 300,000 cases annually in the U.S., the rapid fat degradation that occurs in pancreatitis is triggered by a
pancreatic enzyme called PNLIP. This enzyme can form fatty acids that cause vital body systems like circulation, kidney and lung functions to fail. Dr. Singh says this multisystem failure is much more common in acute pancreatitis than in diverticulitis.
Dr. Singh says obesity, which increases belly fat, also can worsen acute pancreatitis. He says this highlights the role of obesity not just in the development chronic diseases such as diabetes, but also in the development of sudden-onset diseases such as pancreatitis.
Dr. Singh says the study also found that unsaturated fats, such as oleic acid contained in olive oil and recommended by the Food and Drug Administration as being safer for human consumption, actually increase the risk of organ failure. At the same time, PNLIP, the enzyme in the pancreas that breaks down stored fat in fat cells was not abundant in cells specialized for fat storage.
"Our findings open the door to new therapeutic targets to treat pancreatitis and thereby prevent organ failure," says Dr. Singh. "By inhibiting PNLIP, we may be able to prevent severe pancreatitis, avoid prolonged hospitalizations and save lives."