The feeling a limb doesn't belong is linked to lack of brain structure and connection
People with the mental health condition known as body integrity dysphoria (BID) often feel as though one of their healthy limbs isn't meant to be a part of their bodies. They may act as though the limb is missing or even seek its amputation "to feel complete." Now, researchers reporting in the journal Current Biology on May 7 have found that these feelings that a limb doesn't belong are mirrored in the brains of people with this condition.
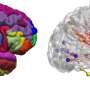
"The feeling that a limb belongs to us relies on the extent to which the sensorimotor limb area is functionally connected to all the other brain regions," says first author Gianluca Saetta, a doctoral student at the University of Zurich. "Crucially involved in this feeling are also the functional connectivity and the density of gray matter in the most crucial area for the representation of how our bodies should look—the right parietal region of the brain."
"Interestingly, we found that the less gray matter in the right parietal region of the brain, the stronger the desire for amputation, and the more BID individuals acted as if they were amputees," Saetta adds. "This simulation behavior helps them to cope with the distressing mismatch between how they want their body to look and how they see it."
To explore the brain mechanisms associated with BID in the new study, Saetta and senior author Peter Brugger of the Psychiatric University Clinic (PUK), Zurich, enrolled 16 men who wanted to remove their healthy left legs and sixteen healthy controls. The question was whether the men with BID would show changes in the brain's functional connectivity or structure—and the researchers found that they did.
Their studies revealed alterations in two key regions associated with BID. The right paracentral lobule (rPCL), which houses the primary somatosensory representation of the affected left leg, showed reduced intrinsic functional connectivity to other parts of the brain, they report. The right superior parietal (rSPL) also showed reduced intrinsic functional connectivity and a reduced concentration of gray matter. That's especially notable because this brain region has been previously identified as a critical hub for body image.
Interestingly, the researchers report, there were no structural alterations evident in the rPCL. In other words, there was no evidence that the men lack the ability to feel or move their left legs.
"We show clear associations between a mental state and changes in brain structure and functionality," Brugger said. "Whether the neural signature of BID comes first and hampers the development of normal limb ownership or whether decades of concern about the lack of such ownership modulate cerebral circuits mediating bodily awareness cannot be answered."
In other words, it's hard to say whether BID leads to a lack of functional connectivity in the brain or vice versa. Nevertheless, the new findings suggest that the desire for amputation in BID individuals may be related to specific anomalies in brain architecture.
The findings show that there's more to BID than has sometimes been suggested. The researchers note that BID is expected to be included in the forthcoming 11th revision of the International Classification of Diseases (ICD-11) as a "disorder of bodily distress or bodily experience." While the condition is considered rare, it's unclear how many people may be affected. After all, Brugger says, it's likely many people with BID don't share this with anyone.
Based on the new findings, the researchers suggest that brain stimulation techniques might hold promise in helping people with BID, a possibility that now warrants further study. Brugger also notes that there are many other variants of BID still to explore and understand better, including people who feel they should be paraplegic or blind.
More information: Current Biology, Saetta et al.: "Neural correlates of Body Integrity Dysphoria" www.cell.com/current-biology/f … 0960-9822(20)30481-4 , DOI: 10.1016/j.cub.2020.04.001