Global study shows four-month treatment for tuberculosis as effective as six-month regimen
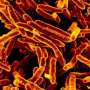
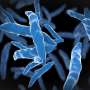
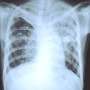
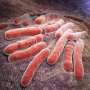
With everyone focused on the ongoing COVID-19 pandemic, it's easy to overlook the fact that there are other health threats still plaguing the world. Number one on the list is tuberculosis (TB), the disease that the World Health Organization calls the leading cause of death worldwide—some 1.5 million fatalities annually—from a single infectious agent (the microbe Mycobacterium tuberculosis). Now, the recently released results of an international clinical trial have shown that a four-month daily treatment plan using a high-dose, or "optimized," course of the drugs rifapentine and moxifloxacin is as safe and effective as the existing standard six-month daily therapy.
The new regimen is the first successful short-course treatment option for drug-susceptible TB disease in 40 years. The findings from the clinical trial that led to its development—with significant involvement from Johns Hopkins Medicine researchers—were announced Oct. 21, 2020, by the research team funded by the U.S. Centers for Disease Control and Prevention (CDC) and the National Institutes of Health (NIH).
In the past 40 years, physicians have put their patients with TB on a six-month treatment regimen, which includes daily doses of the drugs rifampin, isoniazid, pyrazinamide and ethambutol for eight weeks, followed by 18 weeks of daily therapy with just rifampin and isoniazid. Looking for a way to shorten the regimen without sacrificing safety or efficacy, the CDC's Tuberculosis Trials Consortium and the AIDS Clinical Trial Group (funded by the NIH's National Institute of Allergy and Infectious Diseases) conducted one of the largest TB clinical trials in history. It involved more than 2,500 participants, ages 12 and older with newly diagnosed TB, who were enrolled at 34 clinical sites in 13 countries. The trial included 214 people with HIV infection.
Participants in the trial, known as Study 31/A5349, were given standard treatment or one of two four-month drug regimens for their TB—the first featuring high-dose rifapentine, instead of rifampin, and the second using high-dose rifapentine and moxifloxacin.
"We found that four months of treatment—with rifapentine and moxifloxacin—cured TB as well as the six-month standard treatment, had a comparable level of safety, and was well tolerated by patients," says Richard Chaisson, M.D., director of the Johns Hopkins Center for Tuberculosis Research, professor of medicine at the Johns Hopkins University School of Medicine and one of four co-chairs of Study 31/A5349.
However, the regimen of high-dose rifapentine without moxifloxacin was found to be inadequate.
Along with their leadership role in the trial, the Johns Hopkins Medicine researchers followed 100 participants at a Johns Hopkins Medicine-funded center in South Africa and previously had conducted a number of animal studies that helped lay the groundwork for the latest investigation.
"This will certainly change how TB is treated in the United States [which still documents just under 10,000 cases annually] and likely, the world," Chaisson says.