Combined approach could boost breast cancer immunotherapy, study suggests
Activating an immune signaling pathway best known for fighting viral and bacterial infections can boost the ability of genetically engineered T cells to eradicate breast cancer in mice, according to a new study by researchers at the University of North Carolina. The study, to be published December 31 in the Journal of Experimental Medicine (JEM), suggests that CAR T cells, which are already used to treat certain blood cancers in humans, may also be successful against solid tumors if combined with other immunotherapeutic approaches.
Chimeric antigen receptor (CAR) T cells are a type of white blood cell that have been genetically engineered to recognize and attack cancer cells expressing specific proteins on their surface. They have been successfully used to treat patients with B cell lymphomas and are currently undergoing clinical trials for the treatment of many other types of blood cancer. "However, the clinical activity of CAR T cells in patients or animal models with solid tumors has been modest," says Jonathan S. Serody, the Elizabeth Thomas Professor of Medicine, Microbiology, and Immunology and Director of the Cellular Therapy Program at the University of North Carolina School of Medicine.
CAR T cells may be less effective against solid tumors because they have to migrate into the tumors and then survive long enough to kill all of the tumor cells. Moreover, the cells and molecules surrounding tumors are often immunosuppressive, activating an immune checkpoint that causes the CAR T cells to lose their activity.
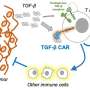
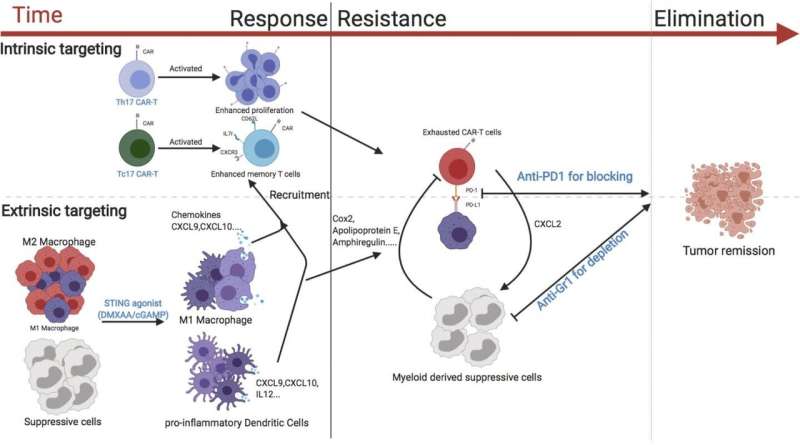
In the new study, Serody and colleagues tested several strategies to boost the effectiveness of CAR T cells in a mouse model of breast cancer. One effective strategy was to simultaneously treat the mice with drugs, such as cGAMP, that activate the STING pathway, an immune cell signaling pathway that normally induces inflammation in response to invading viruses or bacteria. Activating the STING pathway created a proinflammatory environment within the mouse tumors, improving the CAR T cells' ability to accumulate and attack the tumor cells. The accumulation was particularly great when the mice were infused with CAR T cells that produce the immune signaling molecule IL-17A, compared with CAR T cells generated using standard techniques.
Serody and colleagues determined that the CAR T cells' attack could be sustained for longer periods if the mice were also treated with therapeutic antibodies that deplete immunosuppressive cells from the tumor environment and prevent the immune checkpoint from deactivating the CAR T cells. The researchers found that combining all of these approaches led to the complete eradication of breast tumors.
"cGAMP is in clinical trials for the treatment of patients with cancer, there are multiple ongoing clinical trials using approaches to inhibit immunosuppressive cells for patients with malignant disease, and there are clinical trials currently evaluating the combination of CAR T cells with immune checkpoint blockade," Serody says. "Together therefore, our data suggest a viable strategy for boosting CAR T activity in solid tumors."
More information: Nuo Xu et al, STING agonist promotes CAR T cell trafficking and persistence in breast cancer, Journal of Experimental Medicine (2020). DOI: 10.1084/jem.20200844