Scientists reveal how the body controls allergy-causing immune cells
Scientists at the Francis Crick Institute have uncovered biological processes key to regulating immune cells that can cause allergic reactions unless closely controlled.
They hope this insight into an understudied aspect of our immune system could help expose what goes wrong when the body develops allergies or goes into anaphylaxis.
As part of their new study published in Immunity today (Tuesday), the research team performed comprehensive CRISPR genetic screens to identify genes that control the number and differentiation of white blood cells that make IgE antibodies.
IgE antibodies are present at very low numbers in our immune system, and unlike other immune cells are not associated with lasting immune responses. They play a crucial role in recognizing immediate threats like parasites and venoms. But they can also be produced in response to non-threatening environmental substances like pollen and foods, in the case of allergies. And researchers think this happens when IgE antibodies fail to self-limit their production.
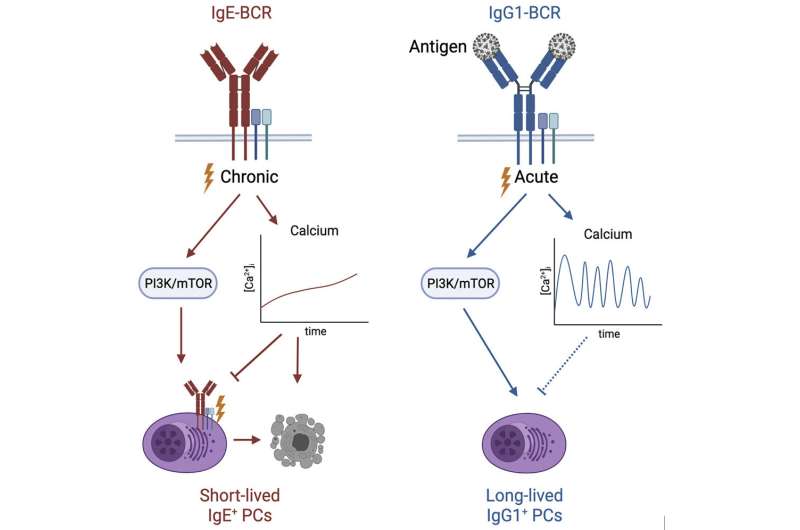
They identified a number of biological pathways associated with the production and survival of white blood cells called B cells that are committed to producing IgE antibodies. In particular, they found that calcium signaling is key to inhibiting the survival of these cells and their differentiation into plasma cells that produce IgE in large quantities.
Pavel Tolar, lead researcher and head of the Crick's Immune Receptor Activation Laboratory, said: "IgE antibodies are associated with acute immune responses like itching skin or vomiting, but when they persist in the blood, they might cause a chronic reaction. We think that for some people, this is what happens in the case of exposure to allergens."
In the lab, the researchers deleted genes associated with calcium signaling in mice and found that the IgE antibody response was increased, confirming calcium's key role in controlling the IgE levels and activity in the body.
"Intracellular calcium is usually associated with an increased immune response," added Pavel. "But in the case of IgE B cells, we see the opposite—it's a limiting factor in their survival. If we can examine calcium levels in B cells in the context of specific allergies, we might be able to find ways to better regulate this overactive immune response."
More information: Rebecca Newman et al, Chronic calcium signaling in IgE+ B cells limits plasma cell differentiation and survival, Immunity (2021). DOI: 10.1016/j.immuni.2021.11.006